- Over 40% of smokers who received one psilocybin dose quit by month 6 versus 10% of nicotine patch users in a pilot randomized trial.
- No serious adverse events were reported, and the most common side effects with psilocybin were temporary increases in blood pressure and nausea.
- Psilocybin works by increasing “mental flexibility,” allowing patients to reframe their relationship with addiction, researcher said.
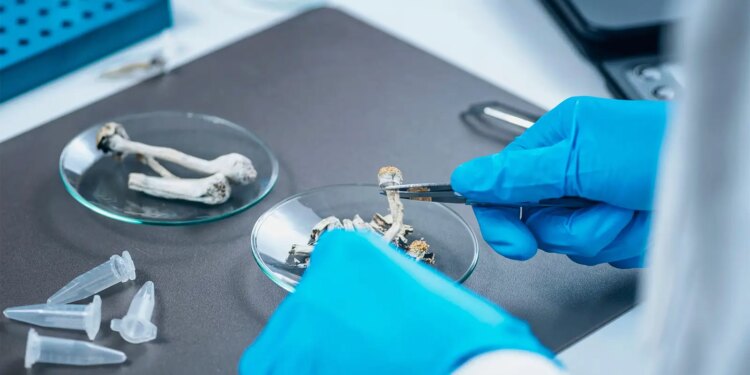
A single high-strength dose of psilocybin was more effective than nicotine patches for helping smokers quit, a pilot randomized trial showed.
When added to cognitive behavioral therapy (CBT), 40.5% of participants who received one dose of psilocybin (30 mg/70 kg) abstained from smoking for 6 months compared with 10% of those who wore a nicotine patch (OR 6.12, 95% CI 1.99-23.26, P=0.003), reported Matthew W. Johnson, PhD, of Johns Hopkins University School of Medicine in Baltimore, and colleagues.
Safety wasn’t an issue, as no serious adverse events occurred. Most adverse events were expected effects with psilocybin such as transiently increased blood pressure, headache, and nausea, the group wrote in JAMA Network Open.
Psilocybin is “a promising candidate for smoking cessation that should move forward in the FDA process toward potential approval,” Johnson and team noted. While researchers are still decoding how psilocybin works, Johnson said it biologically facilitates the psychotherapeutic process.
“The big picture emerging is that psychedelics work through transdiagnostic mechanisms and therefore have broad promise across nominally distinct disorders,” he told MedPage Today. “The mind is put in a temporary state with increased flexibility. That’s the source of the promise and potential risk. People have insights and changes in the way they view themselves and their problems, and these psychological effects often last beyond the acute effects of the drug.”
“It seems that the psychological experience of the ‘trip’ is likely necessary for the therapeutic effects, at least with the treatment models used in this and most psychedelic studies,” Johnson continued. “It’s looking to be a promising treatment for depression, cancer distress, and other disorders.”
Prior data have shown that psilocybin may have benefits in several substance use disorders, but Johnson said the current findings indicated that it “doesn’t just work on addictions associated with hitting rock bottom.”
“Tobacco kills more people than all other addictive substances combined, but it typically doesn’t result in the short-term quality-of-life destruction of many other substances,” he explained. “This suggests it has something to do with addiction, per se, rather than quelling the drug reinforcement or withdrawal of the addictive drug, which is how most addiction medicine works.”
Despite these findings, Johnson warned that the risk and efficacy profile of psilocybin may differ outside of a controlled clinical environment and noted that psilocybin remains a Schedule I substance. “If you are a clinician, keep your eye on this for when it might one day be an available treatment. In the meantime, if patients inquire, be sure to let them know that there are many safety factors at play in this research,” he advised.
This trial included 82 psychiatrically healthy adult smokers, with data collected from January 2015 to May 2023, at the Johns Hopkins Bayview Medical Center. Average age was 47.6, 59.8% were male, and 89% were white. Participants smoked an average of 15.7 cigarettes per day and reported a median of six previous quit attempts.
All participants received 13 weeks of CBT focused on smoking cessation. They were randomized 1:1 and at week 5 to receive psilocybin or a course of nicotine patches.
The psilocybin group received psychoeducation about treatment effects prior to dosing. During the dosing session, participants laid on a couch wearing eye shades, listened to a music program through headphones, and were asked to focus attention inward.
One day after dosing, 90.5% of psilocybin participants and 80% of nicotine patch users abstained from smoking. By day 7, abstinence rates were 52.4% and 25%, respectively (OR 3.30, 95% CI 1.32-8.70, P=0.01). The psilocybin group smoked an average 50% fewer daily cigarettes through month 6.
Adverse events were well-managed. During administration, the psilocybin group’s average peak blood pressure was 160.2/100.9 mm Hg, with a heart rate of 87.6 bpm. One participant required sublingual nitroglycerin to manage hypertension.
“Psychedelic therapy requires few administrations, largely limiting adverse events to supervised sessions,” the researchers pointed out. “In contrast, typical smoking cessation medications are used daily for multiple weeks, resulting in potential for delayed adverse events and adherence issues.”
Some limitations included the trial’s lack of blinding and participant diversity. Nearly 65% of participants reported prior psychedelic use — far higher than the national average of 13.8% — which may indicate recruitment bias.
Source link : https://www.medpagetoday.com/pulmonology/smoking/120236
Author :
Publish date : 2026-03-10 15:00:00
Copyright for syndicated content belongs to the linked Source.