- Using a liver stiffness measurement to screen for liver fibrosis in patients with type 2 diabetes could help identify those at an increased risk of all-cause mortality.
- While liver stiffness measurement emerged as an independent risk factor associated with mortality, the FIB-4 index score did not.
- Noninvasive liver stiffness assessment should be incorporated into routine diabetes management, though access may be limited, the authors said.
Using a liver stiffness measurement (LSM) to screen for liver fibrosis as part of the routine management of patients with type 2 diabetes could help identify those at an increased risk of all-cause mortality, a cohort study suggested.
Among patients with diabetes, LSM emerged as an independent risk factor associated with mortality, with a 6% increase in the hazard of death for each 1-kPa increase in liver stiffness (adjusted HR 1.06, 95% CI 1.04-1.09, P<0.001), after adjusting for age, sex, body mass index (BMI), and HbA1c level, reported Fernando Bril, MD, of the University of Alabama at Birmingham, and colleagues.
An increased risk of all-cause mortality was associated with the coexistence of diabetes with metabolic dysfunction-associated steatotic liver disease (MASLD; aHR 2.77, 95% CI 1.16-6.65, P=0.03) and diabetes with advanced liver fibrosis (aHR 6.41, 95% CI 1.03-39.85, P=0.047), they noted in JAMA Network Open.
“These findings emphasize the urgent need to increase awareness among clinicians and patients about the need to screen for liver disease” in patients with type 2 diabetes, wrote Bril and colleagues, and “support incorporating noninvasive liver stiffness assessment into routine [type 2 diabetes] management to improve risk stratification and identify patients at elevated risk of adverse outcomes.”
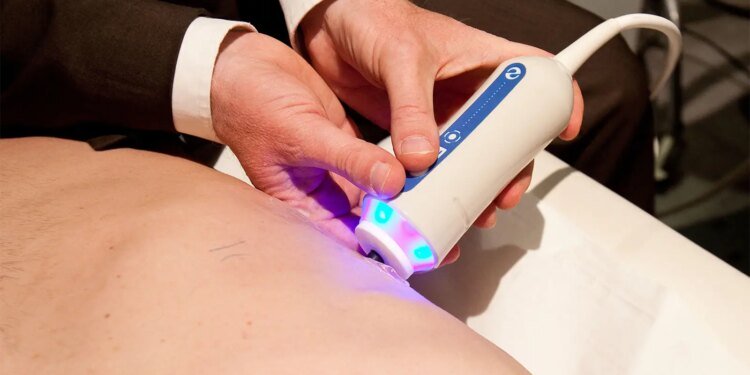
However, LSM is assessed by vibration-controlled transient elastography (VCTE), and limited access to this tool, particularly in rural areas, “remains a challenge,” they pointed out.
People with type 2 diabetes have a substantially increased risk of developing clinically significant fibrosis and cirrhosis, and current guidance from the American Diabetes Association recommends fibrosis screening using the Fibrosis-4 (FIB-4) index, followed by confirmatory testing with LSM or an enhanced liver fibrosis test when FIB-4 values are ≥1.3.
In an accompanying commentary, Emad Qayed, MD, MPH, of the Emory University School of Medicine in Atlanta, noted that the study “highlights important limitations of FIB-4 as a fibrosis risk stratification tool in patients with diabetes.”
While LSM emerged as an independent risk factor associated with mortality, the FIB-4 index score did not.
Based on the FIB-4 index, 60.8% of patients with diabetes in the study would be considered low risk (FIB-4 <1.3) and would not have a VCTE performed. Bril and colleagues reported that by the end of follow-up, the mortality rate was 1.2% in this subgroup, compared with 4.7% in the group with an elevated FIB-4 (HR 4.33, 95% CI 1.50-12.51, P=0.01).
However, 24.1% of patients with a FIB-4 index <1.3 had an LSM that was 8 kPa or greater. These patients had a substantially higher mortality rate of 4% compared with 0.4% among those who had negative results on both tests (HR 21.80, 95% CI 2.07-229.44, P=0.01).
Thus, after adjusting for age, sex, BMI, and HbA1c level, an LSM by VCTE of ≥8 kPa in patients with a negative FIB-4 score was associated with a significant increase in mortality risk (aHR 39.36, 95% CI 4.03-384.74, P=0.004).
“These findings suggest that reliance on FIB-4 as the initial screening tool may result in a substantial proportion of patients with high-risk diabetes being missed,” Qayed wrote. “This may, in turn, exclude patients from emerging pharmacologic therapies for MASLD.”
For their analysis, Bril and colleagues used a representative U.S. cohort from the National Health and Nutrition Examination Survey from 2017 to 2018, including 4,102 patients with a mean age of 47 years; 50.7% were female, 63% were white, 16.3% were Hispanic, 10.7% were Black, and 5.4% were Asian. Mean BMI was 29.5, and 14.5% had diabetes.
Compared with the overall population, patients with diabetes were older, had a worse metabolic profile, and had a higher prevalence of comorbidities.
After a mean follow-up of 24 months, 59 patients died (24 with diabetes). Patients who died during follow-up compared with those who lived were older (mean age 62 vs 47), more likely to be white (85.1% vs 62.7%), had a higher prevalence of diabetes (35.7% vs 14.2%), and a higher HbA1c level (mean 6.2% vs 5.6%).
Among patients receiving diabetes treatments, those who died had a lower use of metformin, pioglitazone (Actos), and GLP-1 receptor agonists, and higher use of insulin.
Source link : https://www.medpagetoday.com/gastroenterology/generalhepatology/120373
Author :
Publish date : 2026-03-18 20:52:00
Copyright for syndicated content belongs to the linked Source.