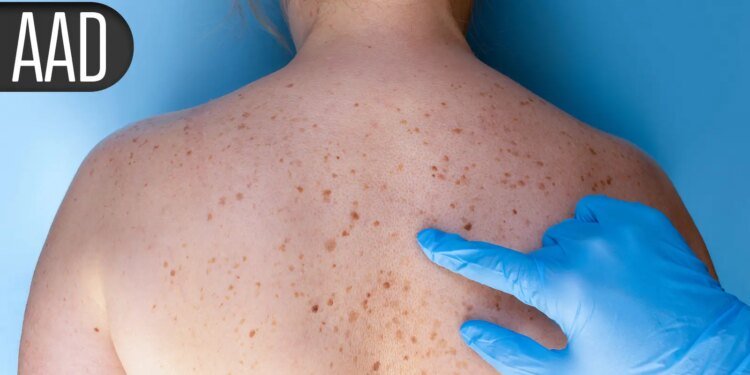
DENVER — Biological agents targeting interleukin-4 receptor alpha (IL-4Rα) in atopic dermatitis (AD) achieved rapid and substantial improvement in up to three-fourths of patients, according to randomized trials from China.
Rademikibart administered every 2 weeks achieved at least 75% skin clearance (EASI 75) at 16 weeks in 74.2% of adults and adolescents with moderate/severe AD. Almost half of the patients met the co-primary endpoint of investigator-assessed clear or nearly clear skin (IGA 0/1) and at least a 2-point improvement from baseline. MG-K10, administered every 4 weeks, achieved EASI 75 status at 16 weeks in 59.8% of patients, and a third of patients met IGA 0/1 criteria with at least a 2-point improvement.
Response rates continued to increase out to 52 weeks, surpassing 90% for EASI 75 in both studies and 77-87% for IGA 0/1, as reported at the American Academy of Dermatology meeting.
“We observed deep clearance of skin lesions and remarkable antipruritic effects at week 16 with rademikibart,” said Cheng Zhou, MD, of Peking University People’s Hospital in Beijing. “Efficacy was durable with long-term treatment, and responses were sustained or further increased through week 52.”
Jianzhong Zhang, MD, also of Peking University People’s Hospital, said MG-K10 “demonstrated robust and durable efficacy … that translated into meaningful quality-of-life benefits… . These results support MG-K10 as a promising therapy for long-term management of atopic dermatitis.”
Credulity-Stretching Results
The historically higher response rates did not go unnoticed by the audience.
“Just so everybody is clear, what you just showed us is 20 to 30 percentage points higher than we’ve ever seen with any drug in AD,” said Andrew Blauvelt, MD, of Blauvelt Consulting in Annapolis, Maryland, following Zhou’s presentation. “I’m kind of shocked at your results given the target, IL-4Rα. What do you think it is about your drug? How is it different from dupilumab [Dupixent], and other drugs we’ve heard about from Chinese investigators, to make the efficacy so much higher? It’s not a little higher. It’s much higher. It’s incredible.”
As an example, three studies of the OX40 ligand inhibitor amlitelimab, reported at the same late-breaking research session, showed investigator-assessed response rates of 21.1% to 32.3% at 24 weeks.
Zhou suggested rademikibart’s molecular design (binding to an epitope distinct from that of dupilumab), resulting in higher affinity for the target, as one possible explanation. Genetic differences and other factors associated with the Chinese population might also be involved.
“Maybe because our weight is not so high,” said Zhou, drawing laughter from the audience. “More studies are needed in other populations.”
April Armstrong, MD, MPH, of UCLA Health in Los Angeles, had similar questions for Zhang about the response rates with MG-K10.
“Inhibition of IL-4 receptor alpha is a well-established pathway,” said Armstrong. “What are some of the key advantages that you see with this new molecule over existing therapies, such as dupilumab?”
Zhang also suggested the molecular design of MG-K10 and factors specific to the Chinese population as potential explanations.
An unidentified member of the audience noted that MG-K10 was associated with a much lower rate of conjunctivitis (2-3%) than what has been reported with other long-acting therapies that inhibit IL-13 (an effect of IL-4Rα blockade).
“Maybe it relates to the molecular modification,” said Zhang. “We will have to watch for this during real-world experience.”
Rademikibart Study
Consistent with other agents that block IL-4Rα, rademikibart and MG-K10 inhibit IL-4 and IL-13 signaling pathways. Rademikibart’s higher affinity for the target leads to effects equivalent to those of dupilumab but at a lower concentration, said Zhou. The drug is under evaluation for asthma and chronic obstructive pulmonary disease, in addition to AD.
Zhou reported findings from the phase III RADIANT-AD trial, which involved patients 12 and older with moderate/severe AD. They were randomized to rademikibart (600-mg loading dose, then 300 mg every 2 weeks) or placebo for 16 weeks, at which point patients in both groups continued maintenance treatment with rademikibart for an additional 36 weeks. The co-primary endpoints of EASI 75 and IGA 0/1 plus ≥2-point improvement were assessed at 16 weeks.
Data analysis included 259 randomized patients. More than twice as many patients in the rademikibart group met EASI 75 criteria at 16 weeks (74.2% vs 34.4%, P=0.0005), and a statistically significant difference emerged at 4 weeks (P=0.005). At the end of follow-up, 96.6% of patients randomized to rademikibart and 95.9% of the placebo-treated patients switched to the IL-4Rα inhibitor met EASI 75 response criteria.
More than twice as many patients in the rademikibart met the co-primary endpoint at 16 weeks (47.7% vs 17.6%, P=0.0005). At 52 weeks, 87.1% of the patients started on rademikibart had IGA 0/1 status and ≥2-point improvement, as did 75.6% of the patients who crossed over to the IL-4Rα inhibitor.
The 16-week EASI 90 response rates were 43.0% with rademikibart and 14.5% with placebo (P=0.0005), increasing to 85.3% and 78.9%, respectively, at 52 weeks. The proportion of patients with at least a 3-point improvement in pruritus score at 16 weeks were 54.7% with rademikibart and 27.5% with placebo (P=0.0005) and 91.2% versus 88.4% at 52 weeks.
Rademikibart had a favorable safety profile at 16 weeks (three ≥3 adverse events [AEs]) and 52 weeks (eight grade ≥3 AEs).
MG-K10 Study
The MG-K10 molecular construct includes an Fc mutation that results in an extended half-life, permitting once-monthly dosing, said Zhang. Administration begins with a 600-mg loading dose, followed by 300-mg dosing every 4 weeks.
The IL-4Rα inhibitor was evaluated in a randomized, placebo-controlled phase III trial involving 499 adults, randomized 2:1 to MG-K10 or placebo for 16 weeks, followed by maintenance MG-K10 for both groups to week 52. The co-primary endpoints were EASI 75 response and IGA 0/1 status (with ≥2-point improvement) at 16 weeks.
The primary analysis showed that 59.8% of patients in the MG-K10 arm had EASI 75 responses at 16 weeks versus 22.9% of placebo-treated patients (P<0.0001). IGA 0/1 response rates were 32.7% versus 7.2% (P<0.0001). At the end of maintenance therapy, EASI 75 response rates did not differ significantly (94.3% vs 90.9%), nor did the IGA 0/1 responses (76.6% vs 73.4%).
EASI 90 response rates at 16 weeks were 33.0% with MG-K10 and 7.8% with placebo (P<0.0001), increasing to 79.1% versus 72.0% at 52 weeks. The proportion of patients with at least a three-point improvement in pruritus score at 16 weeks was 58.0% with MG-K10 and 28.9% with placebo (P<0.0001), increasing to 84.6% versus 84.5% at 52 weeks. Improvement in clinical symptoms translated into statistically significant and clinically meaningful improvement in quality of life at 16 weeks on two different validated instruments, and patients who crossed over from placebo to MG-K10 had similar quality of life scores at 52 weeks.
Serious AEs were infrequent with MG-K10 at 16 weeks (2.1% vs 3.0% for placebo) and 52 weeks (5.1% vs 4.5% for placebo crossover).
Source link : https://www.medpagetoday.com/meetingcoverage/aad/120625
Author :
Publish date : 2026-04-02 21:44:00
Copyright for syndicated content belongs to the linked Source.