Evidence of iatrogenic beta-amyloid transmission was identified in two patients who developed early-onset cerebral amyloid angiopathy decades after undergoing pediatric cardiac surgery.
The findings suggest that the use of cadaveric dura mater patches in cardiac surgery seeded amyloid pathology, leading to neurovascular complications 40 years later, noted Jean-Baptiste Brunet de Courssou, MD, MSc, of University of Versailles Saint-Quentin-en-Yvelines in France, and colleagues.
“We hypothesize that amyloid-beta seeds present in the cadaveric dura mater passed directly into the bloodstream or induced misfolding of circulating plasmatic amyloid-beta, eventually crossing the blood-brain barrier and causing iatrogenic cerebral amyloid angiopathy,” Brunet de Courssou and co-authors wrote in Neurology.
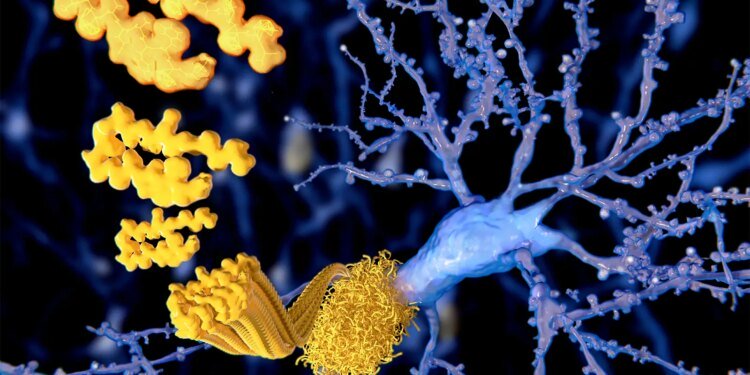
In cerebral amyloid angiopathy, amyloid protein deposits build up in the walls of brain arteries, increasing the risks of hemorrhagic stroke and cognitive decline. Cerebral amyloid angiopathy usually occurs in older adults and is associated with dementia.
The two patients in the case report — a 43-year-old man and a 42-year-old woman — both presented with symptomatic lobar hematomas and imaging features consistent with probable cerebral amyloid angiopathy, Brunet de Courssou and colleagues reported. Amyloid PET imaging showed diffuse brain amyloidosis, with abnormal cerebrospinal fluid amyloid levels in analysis.
Clinical presentations occurred approximately 40 years after surgery for transposition of the great vessels, a rare congenital heart defect in which the aorta and pulmonary artery are switched. The use of cadaveric dura mater during surgery was confirmed in one case and deemed likely in the other. Genetic screening for hereditary causes of cerebral amyloid angiopathy was negative, and both patients were APOE3 homozygotes.
Iatrogenic transmission of amyloid pathology has been reported previously, notably after neurosurgical procedures involving cadaveric dura mater grafts.
“Our cases extend this concept by suggesting that such transmission may also occur in other surgical settings,” said co-author Sandrine Deltour, MD, PhD, also of University of Versailles Saint-Quentin-en-Yvelines.
“This is the first well-documented report of iatrogenic cerebral amyloid angiopathy associated with cardiac surgery,” she told MedPage Today.
“These cases provide evidence that cerebral amyloid angiopathy can be acquired rather than purely sporadic or genetic,” Deltour added. “They support the hypothesis of long-term iatrogenic transmission of amyloid pathology following exposure to cadaveric dura mater grafts.”
Human-to-human transmission of amyloid-beta pathology was first reported in 2015 in patients who died of iatrogenic Creutzfeldt-Jakob disease after being treated with cadaveric human growth hormone.
The first human was followed by reports of early-onset cerebral amyloid angiopathy in patients who had childhood medical procedures using cadaveric dura mater, demonstrating that amyloid-beta transmission could result in disease later in life, said Gargi Banerjee, MD, and David Werring, PhD, of the University College London.
“Several cases have been reported subsequently, with emerging evidence that the clinical phenotype has features unusual for sporadic cerebral amyloid angiopathy (for example, hemorrhagic lesions in non-lobar locations and imaging changes suggestive of vessel leakage or inflammation),” Banerjee and Werring wrote in an accompanying editorial.
While acquired prion diseases are rare, the concept of protein misfolding and propagation may extend beyond classic prion disorders, the editorialists noted.
“The broader biological implications are enormous; the existence of iatrogenic cerebral amyloid angiopathy shows that prions are not necessarily exclusive or peculiar to disorders involving prion proteins and instead that prion biology has direct clinical relevance for other disorders associated with misfolded protein aggregation,” they observed.
“In the case of amyloid-beta, we are in the dark: what exactly is being seeded from these contaminated grafts, where does it go and where does it propagate, and how does it eventually access the brain and leptomeninges? Given reports of iatrogenic Alzheimer’s disease after treatment with cadaveric human growth hormone, and the possibility of amyloid-beta transmission through blood transfusions, these questions have clinical and public health consequences and should be recognized as research priorities,” Banerjee and Werring wrote.
Although cadaveric dura and cadaveric human growth hormone are no longer used, the potential risks of amyloid-beta transmission through blood transfusion or organ transplantation warrant further study, they suggested.
Diagnosing iatrogenic cerebral amyloid angiopathy is challenging, Deltour noted. “What is particularly striking is the very long latency between the surgical procedure and clinical presentation, often spanning several decades,” she said.
“This highlights that patients may present much later in life with intracerebral hemorrhage or cognitive symptoms, and that this etiology can easily be overlooked,” Deltour pointed out. “Our observations emphasize the need for clinicians to carefully investigate remote cardiac surgical histories, especially in relatively young patients with imaging features suggestive of cerebral amyloid angiopathy.”
Source link : https://www.medpagetoday.com/casestudies/neurology/120533
Author :
Publish date : 2026-03-27 20:02:00
Copyright for syndicated content belongs to the linked Source.