SAN JUAN, PUERTO RICO — A negative study in low-grade serous ovarian cancer might have uncovered a pathway toward more effective treatment for a large subgroup of patients, according to the NRG-GY019 trial.
The randomized study established chemotherapy plus letrozole as standard of care for low-grade serous ovarian carcinoma (LGSOC), as letrozole monotherapy failed to meet non-inferiority requirements for progression-free survival (PFS). However, a subgroup analysis showed a 50% reduction in recurrence with single-agent letrozole in patients who had no gross residual disease after surgery. Analysis of that subgroup — comprising almost two-thirds of the patients randomized to letrozole monotherapy — yielded a hazard ratio (HR) within the non-inferiority range.
Median PFS had yet to be reached in either arm and a preliminary analysis of overall survival (OS) showed that more than 90% of patients remained alive after more than 2 years of follow-up. Letrozole alone was much better tolerated, as patients treated with chemotherapy were four times more likely to develop grade ≥3 adverse events (AEs), reported Amanda Fader, MD, of Johns Hopkins Medicine in Baltimore, at the Society of Gynecologic Oncology (SGO) meeting.
“It merits consideration that in the letrozole monotherapy arm, recurrence was markedly higher with any residual disease, approximately double that observed in those patients with no gross residual disease after cytoreductive surgery,” Fader said. “We believe that this disparity likely materially contributed to the inability to establish non-inferiority of letrozole monotherapy versus chemotherapy and letrozole in the intention-to-treat population.”
“This trial, though, is practice defining and establishes, for the first time, a definitive standard of care for patients being treated in the frontline setting with advanced low-grade serous ovarian carcinoma,” she added. “Nevertheless, in a prespecified, hypothesis-generating analysis of patients without gross residual disease, which we know is a better prognostic group … rates of disease progression were not significantly different between treatment arms, and the hazard ratio for progression in the letrozole monotherapy cohort was also relatively favorable. These findings suggest that a clinically relevant subset of patients may be appropriate candidates for letrozole monotherapy.”
‘Biology Matters’
Ongoing follow-up will include intratumoral molecular analyses to provide context for the results and possibly clarify which patients benefit most from chemotherapy and whether letrozole alone may be a reasonable alternative for select patients, said Fader.
NRG-GY019 reflects ongoing efforts to move away from chemotherapy and toward more individualized treatment for LGSOC, said SGO invited discussant Roisin O’Cearbhaill, MD, of Memorial Sloan Kettering Cancer Center in New York City.
“Low-grade serous traditionally has not been well served by chemotherapy,” said O’Cearbhaill. “Although [the study] was stopped early for futility, it may be possible, with careful discussion and patient selection, that there is a subset of patients that we could move away from chemotherapy.”
“We are learning that biology matters,” she continued. “Low-grade serous ovarian carcinoma and endometrioid cancers are distinct entities and should be treated and studied differently. We have learned that there is a certain subset of patients who definitely still require chemotherapy, but great efforts should be ongoing in terms of endocrine and targeted strategies, as these are increasingly viable as early-line options, particularly for younger patients in the early-line setting. Non-chemotherapy approaches used in breast cancer may inform mechanisms of resistance and also activity.”
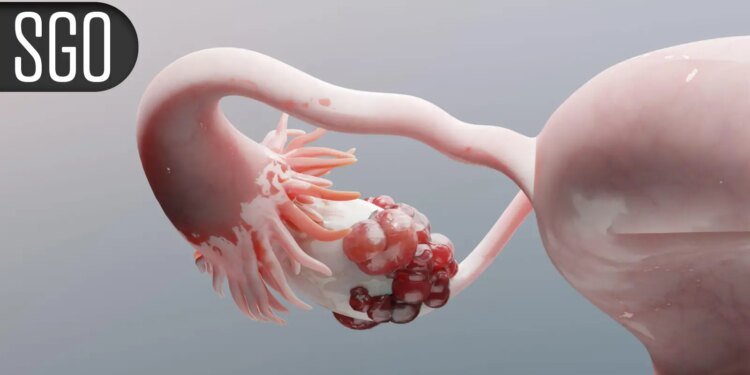
Fader noted that LGSOC is considered a rare cancer accounting for 2-5% of all epithelial ovarian carcinomas and about 10% of SOCs. LGSOC is epidemiologically, pathologically, molecularly, and clinically distinct from high-grade SOC. Historically, patients with either type of SOC have been treated similarly despite clear biologic differences and treatment responses.
LGSOC has an indolent growth rate and is relatively chemoresistant to platinum/taxane therapy, Fader continued. The condition has a high risk of recurrence, and persistent disease after primary cytoreductive surgery has a strong association with worse survival.
About 85-90% of LGSOC expresses estrogen receptors and half express progesterone receptors. Several studies have produced encouraging results with post-cytoreduction endocrine therapy, and the National Comprehensive Cancer Network has endorsed chemotherapy plus endocrine therapy or endocrine therapy alone as a frontline for advanced LGSOC.
“Despite these encouraging retrospective results, prospective randomized data on frontline management have been lacking, until now,” said Fader. “Questions remain about the optimal initial therapy and whether chemotherapy can be omitted without compromising oncological outcomes.”
Key Findings
Eligible NRG-G019 patients had previously untreated stage II-IV LGSOC, p53 wild type, attempted maximal cytoreductive surgery, and no prior chemotherapy. Patients were randomized to receive six cycles of chemotherapy plus oral letrozole daily until disease progression or toxicity or oral letrozole alone for six cycles followed by daily maintenance. The primary endpoint was investigator-assessed PFS in the intention-to-treat (ITT) population.
The trial ended for futility after randomization of 450 patients, and all 450 were included in the ITT analysis. The trial had a prespecified HR for non-inferiority of 1.18 for the comparison of letrozole monotherapy versus paired with chemotherapy. When the trial ended the ITT analysis showed an HR of 1.30.
But the absolute PFS numbers were similar, Fader said, as 77.9% of the chemotherapy group and 71.9% of the letrozole monotherapy arm remained alive and progression free. OS data were immature but showed no significant difference between the treatment arms after a median follow-up of 27.3 months (95% vs 92%).
During the first six cycles of therapy, 46.9% of the chemotherapy group had at least one grade ≥3 AE versus 17.6% with letrozole monotherapy, translating into an odds ratio of 3.99 (95% CI 2.57-6.18, P<0.001).
The prespecified analysis of patients with no gross residual disease after surgery included 286 patients (64% of the total). The analysis showed that 29 of 142 patients had PFS events as did 27 of 144 patients in the chemotherapy arm, a difference that translated into an HR of 1.15. Further inspection of the data showed a recurrence rate of 41.5% with letrozole alone in patients with gross residual disease versus 20.5% in patients with no gross residual disease.
Source link : https://www.medpagetoday.com/meetingcoverage/sgo/120749
Author :
Publish date : 2026-04-12 15:38:00
Copyright for syndicated content belongs to the linked Source.