NEW ORLEANS — Coronary artery calcium (CAC) scoring was disproportionately less reliable as a screen for atherosclerotic plaque for people of certain races and countries, according to the large international study GPS-CAD.
From a real-world imaging database covering 15 countries on six continents and over 32,000 individuals, it was apparent that race/ethnicity and country — considered together as a single surrogate measure for ancestry and environment — was the strongest single predictor of CAC findings, including true positives, where CAC>0 and the coronary CT angiogram (CCTA) was positive for any plaque (AUC 0.62) and false negatives, where CAC=0 but the CCTA was positive (AUC 0.64).
According to Lohendran Baskaran, MBBS, of National Heart Centre Singapore, a false-negative CAC=0 could be predicted by country (being especially prevalent in Egypt, Peru, Canada, Pakistan, Japan, India), race/ethnicity (Middle East, Asian, and Black groups), and age (individuals <55 years).
“In patients with suspected atherosclerotic CAD, decision-making regarding the use of CAC or CCTA, and interpretation of CAC [score]=0 findings should consider race/ethnicity, country and age,” he said at the American College of Cardiology (ACC) annual meeting.
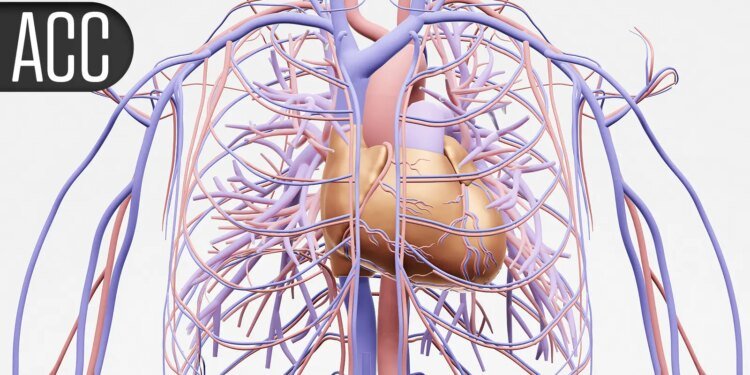
Indeed, a CAC scan measures the amount of calcified plaque in the coronary arteries, and has been previously shown to miss early noncalcified atherosclerotic lesions that are evident on CCTA.
The GPS-CAD investigators had for their study a large cohort of people who’d undergone CCTA and CAC scans to rule out atherosclerotic coronary artery disease (CAD). There were 55% who wound up with a CAC>0 and 60% with any stenosis detected on CCTA.
Most patients had a true positive (53.1%, CAC+, CCTA+) or a true negative (38.2%, CAC-, CCTA-). A minority had false negatives (7.0%, CAC-, CCTA+) and to an even lesser extent, false positives (1.4%, CAC+, CCTA-).
“I was struck by the fact that only 7% of patients had any noncalcified plaque with a score of zero,” though this “obviously varied quite a bit by different race and ethnicity,” commented ACC session panelist Matthew Budoff, MD, of UCLA Medical Center in Los Angeles.
Budoff cited the recent endorsement of CAC scoring in the recent American lipid guideline update as part of decision-making to start lipid-lowering therapy in adults at intermediate risk and select adults at borderline risk with no prior atherosclerotic cardiovascular disease (class I).
“Now that we just have these new cholesterol guidelines from literally just a week ago … I do think that this very low prevalence of calcified plaque volume of these patients with [CAC] scores of zero across all different races and ethnicities really helps reinforce the potential use of that tool,” Budoff said.
“I think anytime we can see populations that span so many countries and so many patients, over 32,000 patients, it really helps us understand the epidemiology of a lot of these diseases. I think [GPSCAD] does strongly reinforce what we would consider the power of [CAC=0],” he stressed.
GPSCAD relied on a pooled dataset composed of data from clinical registries, databases, randomized control trials, and observational studies.
Participants had an overall median age of 59, 45% were women, and 73% were symptomatic. By race and ethnicity, the cohort was 39% non-Hispanic/Latino white, 29% Hispanic/Latino white, 5% Black, 20% Asian, and 4% Middle Eastern.
A finding of CAD, with at least 50% stenosis, was eventually shown in 18% on CCTA.
Baskaran noted that sex, symptom status, and diabetes status had no apparent bearing on the likelihood of a false negative CAC scan.
The GPS-CAD study had its design and rationale paper simultaneously published in JACC: Asia.
The study is still welcoming more contributors and cohort collaborators in its quest to inform pretest probabilities for CAC in specific ethnic groups (e.g., South Asians and Southeast Asians vs East Asians), Baskaran told the room at ACC.
“This extensive and representative dataset provides an essential foundation for developing robust, generalizable [pretest probability] models that account for global ethnic and geographic variations. The geographic distribution of the study sites achieves comprehensive global coverage, with enhanced representation from regions that have been historically under-represented,” according to Junjie Yang, MD, and Ran Xin, MD, both of Chinese PLA General Hospital in Beijing.
“The era of globalization in healthcare has already begun and its momentum is irreversible,” the duo wrote in an accompanying editorial. “It is hoped that the GPSCAD study will significantly contribute to global CAD risk assessment in the era of [artificial intelligence].”
Source link : https://www.medpagetoday.com/meetingcoverage/acc/120547
Author :
Publish date : 2026-03-29 19:40:00
Copyright for syndicated content belongs to the linked Source.