- GLP-1 and GIP agonist users who continued treatment until the time of endoscopy had higher rates of retained stomach contents than those who skipped their last dose.
- Following a clear liquid diet the day before endoscopy eliminated significant residual gastric volume, regardless of GLP-1 drug hiatus.
- Point-of-care ultrasound may be an option to prevent rescheduling these patients.
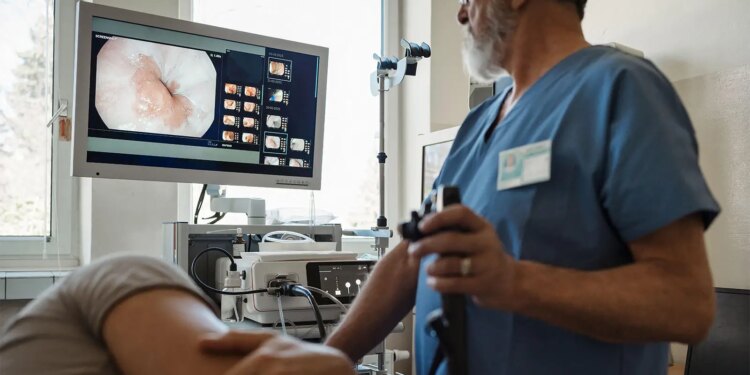
Patients on GLP-1 or GLP-1/GIP agonists had significant residual gastric volume (RGV) if the medication wasn’t held prior to upper endoscopy unless they were on a clear liquid diet the day before, the OCULUS randomized trial showed.
After following standard pre-anesthesia fasting instructions, 25% of patients who continued their GLP-1 drug as usual had clinically significant RGV compared with 3.1% of those who skipped their last dose before sedation (absolute difference 21.9%, 90% CI 7%-36.7%, P=0.003), reported Tilak Shah, MD, MHS, of Cleveland Clinic Florida in Weston, and colleagues.
Clinically significant RGV was defined as a composite of gastric contents that precluded endoscopic examination, required premature termination or endotracheal intubation, and/or resulted in an aspiration event that necessitates extended observation or monitoring, unplanned therapeutics, or hospital admission.
All such cases in this study precluded endoscopic examination, the team noted in JAMA Internal Medicine. No cases resulted in aspiration or unplanned intubation.
“The risk of retained gastric contents in patients who follow standard fasting recommendations is high. Our results would suggest that patients who did not hold at least one dose of the medication prior to surgery or endoscopy should be rescheduled,” Shah told MedPage Today.
“Point-of-care ultrasound could be investigated as an option to prevent rescheduling in these patients,” he continued. “Another option is to reschedule the procedure for the following day with clear liquids if the procedure is required urgently.”
The rate of clinically significant RGV in GLP-1 drug continuers was higher in the subgroup of 35 patients who underwent only upper endoscopy (46.7% of continuers vs 5% of holders, P=0.001). The near 50% rate in continuers “was far higher than we anticipated,” Shah noted.
In contrast, no RGV events occurred in a subgroup of 25 patients who underwent both endoscopy and colonoscopy, regardless of whether they held their GLP-1 agent. These patients followed a clear liquid diet and bowel preparation prior to the procedure. Whether these medications increase the likelihood of an inadequate bowel preparation remains controversial, Shah acknowledged, which is the focus of his team’s ongoing OCULUS-2 trial.
In 2024, the American Society of Anesthesiologists (ASA) stated that most patients shouldn’t stop taking GLP-1 drugs prior to elective surgery — a stark reversal of its 2023 guidance, which advised a 1-week hold for injectables and a 1-day hold for oral agents. Because GLP-1 medications slow gastric emptying, retained gastric contents could increase the risk for regurgitation and pulmonary aspiration while under general anesthesia.
Current recommendations suggest patients can continue medication up until the day of surgery but should follow a liquid diet for 24 hours prior, depending on specific circumstances. “Our study adds further evidence to validate these recommendations, as none of the patients who consumed clear liquids on the day prior had retained gastric contents,” Shah noted.
The ASA guidance also states the presence of gastrointestinal (GI) symptoms, like nausea and constipation, is indicative of delayed gastric emptying, but the researchers found no link between symptoms and retained gastric content. “In fact, all of the patients with retained solid food were without any upper GI symptoms,” said Shah. Only one patient reported nausea and vomiting, and that individual did not have increased RGV.
“Our study questions the validity of considering symptoms in decision-making,” Shah added.
The single-masked, noninferiority OCULUS trial was conducted at two tertiary care centers in the Cleveland Clinic system. It recruited 68 patients scheduled to undergo esophagogastroduodenoscopy, endoscopic ultrasonography, or endoscopic retrograde cholangiopancreatography between July 2024 and May 2025.
Average age was 63, about half were female, and most were taking injectable semaglutide (Ozempic, Wegovy) or tirzepatide (Mounjaro, Zepbound). GLP-1 holders went medication-free for 7-13 days for weekly medications or at least 1 day for daily medications. Continuers took their medication at their usual dosage and schedule.
Among patients on a weekly medication, those who held their dose for more than 3 days were significantly more likely to have a clear stomach than those who held 3 days or less (92.7% vs 62.5%, P=0.047).
The one patient in the hold group who had clinically significant RGV was on daily oral semaglutide (Rybelsus).
Patients who had gastroparesis risk factors other than diabetes were excluded, which may limit generalizability. The study also wasn’t powered to detect differences among individual GLP-1 medications or varying doses.
Source link : https://www.medpagetoday.com/gastroenterology/generalgastroenterology/120325
Author :
Publish date : 2026-03-16 19:51:00
Copyright for syndicated content belongs to the linked Source.