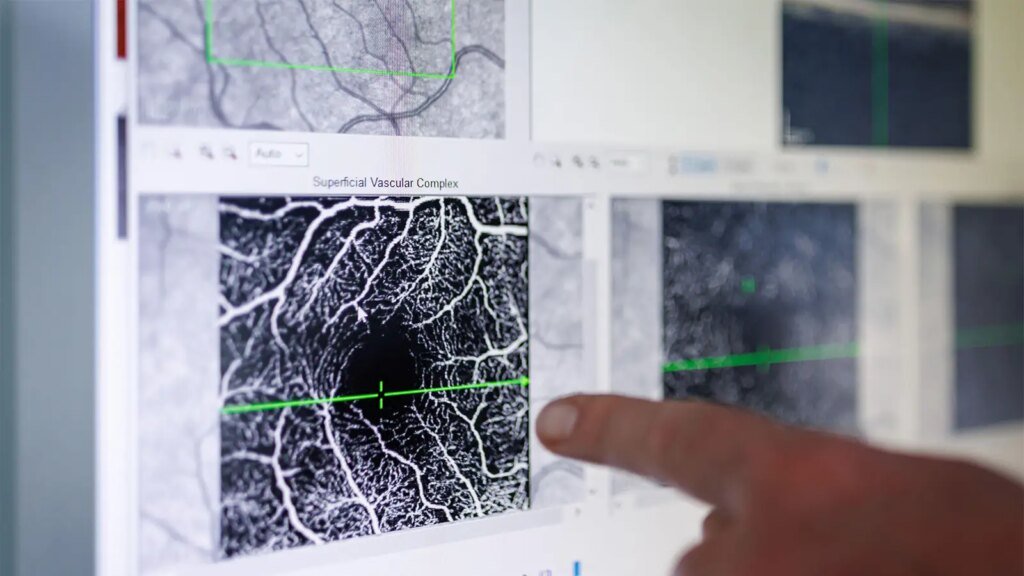
- A prospective study found that the double-layer sign on optical coherence tomography (OCT) was an unreliable surrogate for non-exudative macular neovascularization.
- Clinicians should use OCT and OCT angiography together, rather than relying solely on OCT characteristics to identify underlying non-exudative macular neovascularization, the findings suggested.
- Ophthalmologists should recognize the need to tailor use and interpretation of imaging data to the individual patient, authors of an editorial said.
A key imaging finding in the fellow eye of patients with unilateral neovascular age-related macular degeneration (nAMD) proved to be less accurate for predicting an nAMD precursor than generally accepted, according to angiographic assessment of 550 cases.
By optical coherence tomography (OCT), 20% of fellow eyes had double-layer sign (DLS), often considered a surrogate for non-exudative macular neovascularization (neMNV). OCT angiography (OCT-A) subsequently showed that only 40% of the eyes with DLS had neMNV. The results suggest that DLS on OCT is not a surrogate for neMNV in the fellow eyes of patients with new-onset nAMD, reported Sobha Sivaprasad, MD, of Moorfields Eye Hospital in London, and colleagues.
“Although 20% of fellow eyes of unilateral new-onset [nAMD] have DLS, only 8.6% have neMNV, highlighting the need to diagnose neMNV using OCT-A [rather] than rely on the characteristics of DLS,” the authors concluded in JAMA Ophthalmology. These observations may partly explain interindividual variations in rate of transition to exudative nAMD in the fellow eyes of people with unilateral nAMD on anti-VEGF therapy.”
The study identified a potential conflict of interpretation with multimodal imaging of optical structures and vasculature and has important implications for daily clinical practice and clinical trial design, according to an accompanying editorial.
“For daily practice, the authors suggest that reliance on the DLS alone may be insufficient,” stated Ian C. Han, MD, and Noor-Us-Sabah Ahmad, MD, both of the Institute for Vision Research at the University of Iowa in Iowa City. “Clinicians should not assume the presence of neMNV simply because a DLS is seen on OCT and instead should consider supporting evidence from OCT-A in cases of suspicion. For clinical trials investigating preventive therapies for exudative AMD, enrollment into trials based on the presence of a DLS alone may result in a majority of participants without underlying neMNV, potentially diluting treatment effects.”
However, the study had several limitations that could complicate interpretation, beginning with the small number of study participants — 47 — with neMNV, Han and Ahmad continued. Scan protocols across study sites were not uniform, and graders had the freedom to manually adjust automated layer segmentation boundaries on OCT-A to aid in identifying neMNV. Finally, the study involved images from spectral-domain OCT-A, which is widely available, but prior studies used swept-source OCT-A, which achieves better penetration with reduced signal attenuation and may be better suited for detecting neMNV.
Ideally, OCT and OCT-A should be used in concert, supplemented by other data such as fluorescein angiography for equivocal cases, according to the editorialists.
“Since multimodal imaging is not always available in daily practice, clinicians must recognize the importance of tailoring the use and interpretation of unimodal imaging data for each individual patient,” wrote Han and Ahmad. “In reality, the recognition that every patient has complexity remains most artful. Understanding the gray zones of interpretation … helps us not only to appreciate these complexities in daily practice, but also to inspire us toward the identification of new imaging features or technologies that may be even more informative in the future.”
OCT-A-detected neMNV is a significant risk factor for nAMD and may arise at any stage of non-nAMD, Sivaprasad and colleagues noted. Estimated prevalence of neMNV in prior studies has ranged from 6.25% to 27%. Additionally, recent risk models of neMNV as a predictor of new-onset active nAMD have varied widely.
Prior studies have generally evaluated prevalence of DLS on OCT of the fellow eye as a surrogate for neMNV because OCT of the fellow eye is routine clinical practice when treating the first eye for nAMD, the authors stated. Heterogeneous reflectivity of DLS content is presumed to be a sign of neMNV. However, multiple factors can influence interpretation of DLS content, raising questions about the reliability of DLS as a surrogate for neMNV.
Investigators in the multicenter EYENEON study evaluated the prevalence of neMNV and DLS in fellow eyes of patients with new-onset unilateral nAMD. Data analysis included 550 patients who had both OCT and OCT-A of the fellow eye performed within 30 days of starting anti-VEGF therapy. The primary outcome was prevalence of neMNV in the fellow eye.
The study population had a mean age of 78, and women accounted for 57% of the patients. The data showed that 20.4% of fellow eyes had DLS by OCT, which was more common in female patients (24.1% vs 15.3%, P=0.02) and 8.5% had neMNV by OCT-A at baseline. Mean age did not differ significantly between patients with and without neMNV, although neMNV was more common in patients younger than 65 (22.7%) as compared with patients 65 to 80 years (7%) and those older than 80 (9.1%).
Loss of ellipsoid layer/external limiting membrane and presence of hyperreflective foci were associated with increased odds of DLS (OR 2.51, 95% CI 1.40-4.47, P=0.002 and OR 2.61, 95% CI 1.68-4.06, P<0.001). Presence of neMNV was not associated with any OCT characteristics. Thick DLS occurred more often in eyes with neMNV than in those without neMNV (85.7% vs 55.7%, P=0.002).
Please enable JavaScript to view the comments powered by Disqus.
Source link : https://www.medpagetoday.com/ophthalmology/generalophthalmology/120966
Author :
Publish date : 2026-04-27 15:07:00
Copyright for syndicated content belongs to the linked Source.