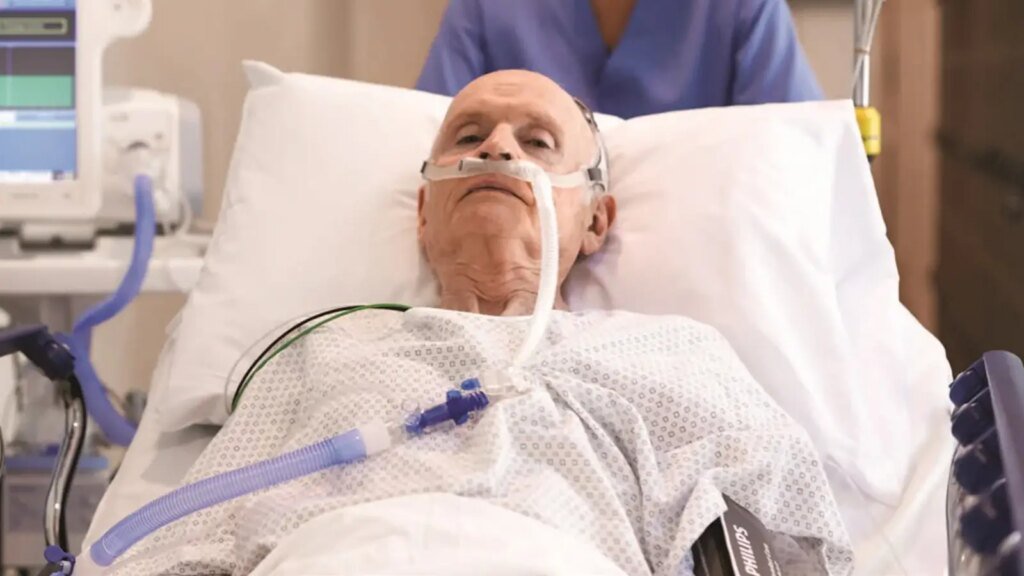
- High-flow nasal oxygen therapy has been increasingly used for noninvasive respiratory support after cardiac surgery.
- In the large randomized NOTACS trial, high-flow nasal oxygen therapy didn’t improve survival with maintenance of functional independence after cardiac surgery in high-pulmonary-risk patients as compared with standard oxygen.
- The findings suggest no need for routine provision of high-flow oxygen in this setting, although use for selected patients was not ruled out.
High-flow nasal oxygen therapy didn’t improve survival with maintenance of functional independence after cardiac surgery in high-pulmonary-risk patients, the NOTACS trial showed.
Whether patients received at least 30 L/min oxygen from the time of extubation or the standard 2-6 L/min, the vast majority of patients spent none of the first 90 days alive and at home (DAH90) without increased functional support compared with baseline.
For that primary trial outcome measure, the median was 0 in both groups (P=0.75), although a minority of patients clustered in the 75-87 day interquartile range, found researchers led by Andrew A. Klein, MBBS, of the Royal Papworth Hospital NHS Foundation Trust in Cambridge, England.
The trial provides “high-quality evidence that a clinically important benefit from prophylactic HFNOT [high-flow nasal oxygen therapy] in this population is unlikely,” the group wrote in JAMA Network Open. “These findings do not support routine implementation of prophylactic HFNOT following cardiac surgery.”
Although high-flow oxygen therapy requires specialist equipment, it has been increasingly used for noninvasive respiratory support in this setting, “despite uncertainty about whether its physiologic effects translate into clinical benefits or reductions in healthcare resource use,” the researchers wrote.
With 1,280 patients randomized in the NOTACS trial, it was larger than all the previous mostly single-center trials examining high-flow oxygen therapy after cardiac surgery and the pilot randomized trial that suggested reduced hospital stay and intensive care unit (ICU) readmission in high-risk groups. But consistent with a meta-analysis of those prior trials, high-flow oxygen increased oxygenation without consistent clinical benefits.
“That systematic review found a decrease in treatment escalation with HFNOT that we did not observe and no difference in the rates of tracheal reintubation, mortality, or hospital or ICU stay that we also observed,” Klein’s group wrote.
The trial follows largely negative findings for high-flow oxygen therapy in patients with acute hypoxemic respiratory failure in the SOHO trial, which found no survival benefit although less intubation within 28 days compared with standard nasal prong oxygen.
Thus, NOTACS “aligns with a broader pattern seen across recent high-flow oxygen trials, where physiological benefits do not necessarily translate into improvements in distal outcomes such as survival or global recovery,” commented Ary Serpa Neto, MD, PhD, of Monash University in Melbourne, Australia, who was not involved with the trial. “In this context, expecting a short exposure to [high-flow oxygen] in the immediate post-operative period to meaningfully alter quality of life is likely unrealistic.”
“That said, there is a consistent signal, both in NOTACS and in prior trials, that high-flow oxygen may reduce postoperative pulmonary complications or the need for escalation of respiratory support, outcomes that are more directly linked to the interface and its physiological effects,” he added. “Taken together, these data suggest that high-flow oxygen should not be used routinely after cardiac surgery, but rather selectively in patients at higher risk of respiratory deterioration or early hypoxemia, where preventing escalation of support or improving comfort remains a clinically relevant and mechanistically coherent goal, even in the absence of an effect on broader outcomes.”
The trial spanned 17 cardiac surgery centers across three countries, enrolling adults undergoing elective or urgent (not emergent) cardiac surgery with cardiopulmonary bypass who were at elevated risk for pulmonary complications due to chronic obstructive pulmonary disease, asthma, lower respiratory tract infection in the prior 4 weeks, a body mass index of 35 or greater, or currently or recently smoking for longer than 10 pack-years.
For the intervention, high-flow oxygen was started at 40% inspired oxygen at a flow of 30 L/min then increased to 50 L/min for 5 to 10 minutes. Standard oxygen therapy was 30-40% inspired oxygen at a flow of 2 to 6 L/min via nasal prongs or nonrebreathing mask without added humidity or heat. If oxygen saturation was less than 93%, oxygen was uptitrated per protocol in both groups. The protocol guided treatment escalation if the patient deteriorated as well.
The intervention was to be followed for at least 16 hours following tracheal extubation whether in the ICU or a hospital ward with an interruption of no more than 1 hour in total for physiotherapy, mobilization, or transfer around the hospital. After that point, ongoing adherence with the allocated oxygen therapy was encouraged.
Limitations included refinement of the primary outcome throughout the trial, although the final version had been prespecified prior to database lock, and none of the secondary outcomes showed differences between treatment groups, including activities of daily living or quality of life measures.
Please enable JavaScript to view the comments powered by Disqus.
Source link : https://www.medpagetoday.com/surgery/thoracicsurgery/120696
Author :
Publish date : 2026-04-08 15:29:00
Copyright for syndicated content belongs to the linked Source.