A non-ablative treatment for benign prostatic hyperplasia (BPH)/lower urinary tract symptoms (LUTS) achieved durable improvement in urinary symptoms and flow rate, according to data from three clinical trials.
Improvements after treatment with the Optilume catheter system persisted out to 3 years, including a 56% reduction in symptoms and a near-doubling of urinary flow rate (Qmax). Only six of 100 patients randomized to the device required surgical retreatment, reported Steven Kaplan, MD, of the Mount Sinai Health System in New York City, at the European Association of Urology (EAU) meeting in London.
“Perhaps we should rethink what we are doing with BPH,” said Kaplan. “You’re not removing a molecule of tissue, and yet the flow rate improvement is similar to when you’re removing tissue … . Perhaps changing the configuration, changing the shape of the prostate is really what we’re actually doing. Some things to think about for [development of] future therapies.”
A second EAU presentation involved pooled data from two prospective, multicenter studies of the Optilume device. The key finding was similar improvement in symptoms and urinary flow regardless of baseline prostate volume, using a cutoff of 50 g, said Kevin Zorn, MD, of BPH Canada in Montreal.
Additionally, a small real-world study conducted in Canada showed outcomes similar to those of the prospective clinical trials.
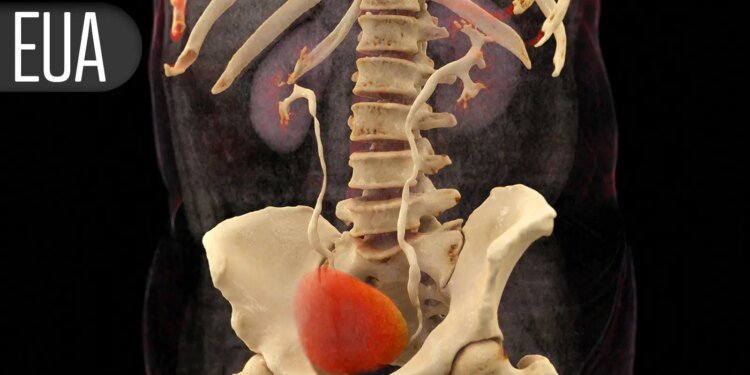
Unlike other minimally invasive treatments for BPH/LUTS, the Optilume system does not remove prostate tissue. Instead, the operator inserts a catheter into the urethra and inflates a paclitaxel-coated balloon to create separation between the two lobes of the prostate, producing an anterior commissurotomy that maintains separation. Continuous release of paclitaxel from the balloon prevents hyperplastic response to maintain patency and improve urinary flow.
Kaplan reported updated results from the randomized (2:1), sham-controlled PINNACLE study. The primary analysis showed numerical improvement at 1 year in the International Prostate Symptom Score (IPSS) and statistically significant improvement in Qmax with Optilume versus 3-month results with the sham procedure.
Updated results for the Optilume arm showed that the mean IPSS score declined from 23.4 to 10.3 at 3 years, whereas Qmax improved from 8.9 to 17.1 mL/s. Surgical retreatment at 3 years consisted of laser in two cases, transurethral resection in two, and prostatic artery embolization and prostatic urethral lift in one patient each.
“The commissurotomy is real, if you do it correctly, and it’s almost impossible not to do it correctly,” said Kaplan. “[The procedure is] actually pretty easy, and in our office, we either use a prostate block or propofol [for anesthesia]. It’s very doable and similar to what we did with TUNA [transurethral needle ablation] and microwave in the past.”
At the 2025 American Urological Association meeting, Kaplan reported 5-year results from the prospective, multicenter EVEREST study of the Optilume system, conducted in Latin America. With longer follow-up, the results in 80 patients were similar to the PINNACLE study, including IPSS improvement from 22.3 to 11.0 and Qmax increasing from 10.9 to 17.8 mL/s.
Zorn reported findings from a pooled analysis of Optilume-treated patients in the EVEREST and PINNACLE studies, focusing on the influence of prostate volume on outcomes. The analysis included a total of 178 patients treated with the device. Patients with a prostate volume ≥50 g had a mean value of 61.9 g, as compared with 34.1 g for men with prostate volumes <50.
After 3 years of follow-up, mean IPSS score had declined from 24.1 to 10.5 in men with larger prostates and from 22.5 to 9.9 in the group with prostates <50 g. Urinary flow improved regardless of baseline prostate volume, although men with smaller organs had numerically greater improvement: 10.0 to 17.6 mL/s versus 9.3 to 13.7 mL/s, which likely reflected better bladder function in men with smaller prostates, who were also younger, said Zorn.
Complication rates and quality of life (QoL) scores also did not differ significantly by baseline prostate volume.
The system also was evaluated in a real-world setting at five sites in Canada — a study to see whether results held up outside of a clinical trial. Data analysis included 30 men with symptomatic BPH and a mean prostate volume of 48.5 mL. Investigators assessed IPSS, QoL, Qmax, and post-void residual (PVR) at baseline and then at 3, 6, and 12 months, said Dean Elterman, MD, of the University of Toronto.
Baseline, 3-month, and 12-month outcomes were as follows:
- IPSS: 23.4, 12.2, 10.8
- QoL: 4.7, 2.3, 2.0
- Qmax: 8.7, 15.9, 14.7 mL/s
- PVR: 95.7, 55.5, 63.1 mL
Hematuria was the most common postoperative event (15 patients), which required cystoscopy with clot evacuation in one case and overnight hospitalization with irrigation in another. Other adverse events were mild dysuria (five patients), urinary retention (seven patients, resolved without incident in all cases), and one case each of urinary tract infection, retrograde ejaculation, and hyponatremia.
Sexual function did not change significantly from baseline to 24 months.
“As we would want to see in a tightly controlled clinical trial, we are seeing the same types of results in a real-world study,” said Elterman. “In this real-world study, the Optilume demonstrated safety and sustained improvements in outcomes.”
Source link : https://www.medpagetoday.com/meetingcoverage/eau/120385
Author :
Publish date : 2026-03-19 18:11:00
Copyright for syndicated content belongs to the linked Source.