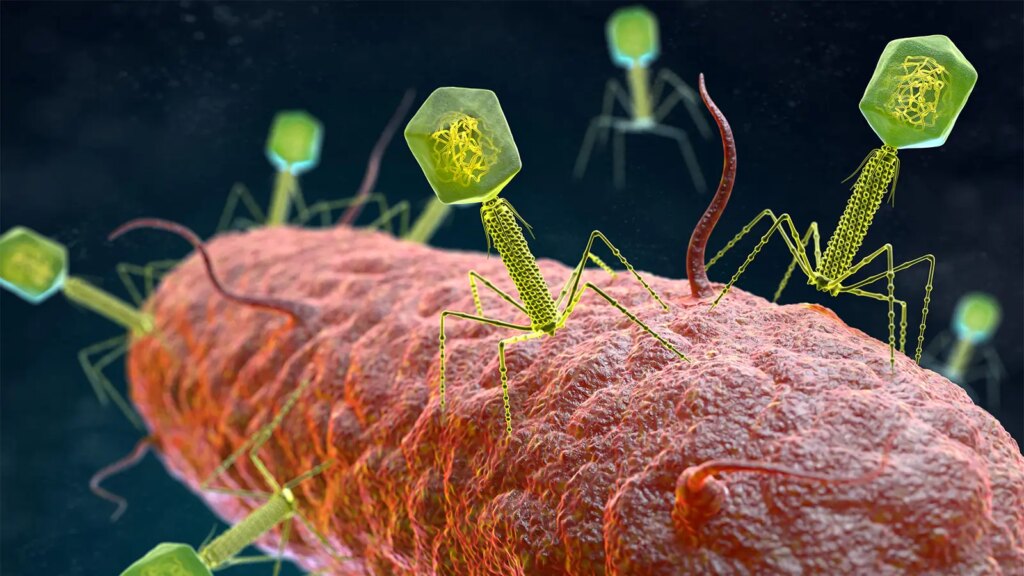
- Bacteriophages (phages) are viruses that kill bacteria.
- Phage therapy used as an experimental therapy in 51 cystic fibrosis patients with multi-drug resistant infections showed that most had a reduction in their microbial load and improvement in lung function.
- Safety appeared good, with no clear cases of serious adverse events from the phages.
For cystic fibrosis (CF) patients with multi-drug resistant (MDR) bacterial infections, experimental treatment with bacteriophage (or phage) has yielded good results with apparent safety so far, a systematic review found.
Across the 51 cases reported, 68% had microbiological response, with some cases of complete eradication. Lung function improved in 74% and by more than 5% forced expiratory volume in 1 second in 12 of the 51 patients, Elena Chiappini, MD, PhD, of the University of Florence and Meyer Children’s Hospital IRCCS in Italy, and colleagues reported in the International Journal of Infectious Diseases.
Most recipients of these viruses that kill bacteria had no adverse events (41 of 52), and only two severe adverse events were reported, “with uncertain association with phage therapy,” Chiappini’s group wrote.
“These results suggest good concordance between microbiological and clinical outcomes, indicating that phage therapy may provide tangible respiratory benefits that extend beyond microbial clearance,” they suggested. “The available evidence supports phage therapy as an innovative option capable of addressing some of the limitations of conventional antibiotics.”
Not only do phage penetrate bacterial biofilms that block conventional antimicrobials, but they also can be directly delivered by inhalation and might act synergistically with antibiotics and reduce the excess airway inflammation that drives disease progression in CF, Chiappini and colleagues noted.
“It seems like the most promising alternative to antibiotics,” Steffanie Strathdee, PhD, of the University of California San Diego and co-director of its Center for Innovative Phage Applications and Therapeutics. “There’ve been really great results coming out of these individual case reports and case series. It’s just that we need the trials to really convince bodies like the FDA … There’s a dire need because there are so few antibiotics in the pipeline.” She was not involved in the review, although some of the studies done at her center were included in the analysis.
The systematic review included 19 English-language studies with CF patients receiving phage therapy for multi-drug resistant infections. Across the 11 case reports, six case series, and two clinical trials, 52 treatment regimens were administered to 51 patients with CF (one got an initial course for Staphylococcus aureus and a separate course later for Pseudomonas aeruginosa).
About half of the patients got single-phage treatment, while 48% got cocktails of two to six distinct phages. Route of administration can include nebulized, intravenous, intrabronchial, and even topical, but it was most often nebulization in the studies (48.1% of cases), followed by exclusive IV administration (30.8%).
Adults represented about 70% of the cases, but the 15 patients under 18 years of age appeared to have at least as good of safety and efficacy from phage treatment.
The most common target pathogen was P. aeruginosa (46.2%), followed by Mycobacterium abscessus (28.8%) and Achromobacter and Burkholderia species (9.6% each). All the studies involved phages with known activity against the implicated bacterial species, with 73.7% selecting phages from pre-established phage libraries or external sources, while the rest directly isolated phages from the patients’ samples.
Subgroup analysis of pathogen type suggested more favorable clinical outcomes from phage treatment in infections caused by P. aeruginosa and Achromobacter species (92% and 80%, respectively) but a lower response rate in M. abscessus (40%).
Treatment lasted a median of 14 days but the substantial variability reflected the lack of standardized therapeutic protocols in this emerging field, as the researchers noted.
Mild adverse reactions reported in two studies included weight loss in one case and subjective fever and fatigue in a handful of patients. The two serious adverse events reported involved an apical pneumothorax in one case, “most likely associated with the bronchoscopic administration procedure rather than the therapeutic agent itself,” and a lung transplant recipient with rapidly deteriorating clinical status for which phage-mediated cytokine release could not be definitively ruled out. The researchers deemed these severe adverse events as “rare but worthy of attention.”
“Although the available data derive from a limited number of cases, our evidence suggests that phage therapy may be generally safe and well tolerated,” they suggested. “Considering protocol heterogeneity and small sample sizes, these findings support further well-designed studies to optimize safety and efficacy.”
Strathdee agreed, noting that CF is driving the field of phage therapy forward for the wide variety of potential uses, such as chronic urinary tract infections or persistent prosthetic joint infections.
Along with trials, resources and coordination are going to be key determinants of how phage therapy progresses, she added. “What we really need are phage libraries that are large enough and well characterized that have phage to tackle the most common and most pernicious superbugs,” she told MedPage Today. “And right now, it’s like having a million keys scattered around the world and a million locks scattered all around the world, and you don’t know which key matches which lock.”
Please enable JavaScript to view the comments powered by Disqus.
Source link : https://www.medpagetoday.com/pulmonology/cysticfibrosis/120522
Author :
Publish date : 2026-03-27 15:37:00
Copyright for syndicated content belongs to the linked Source.