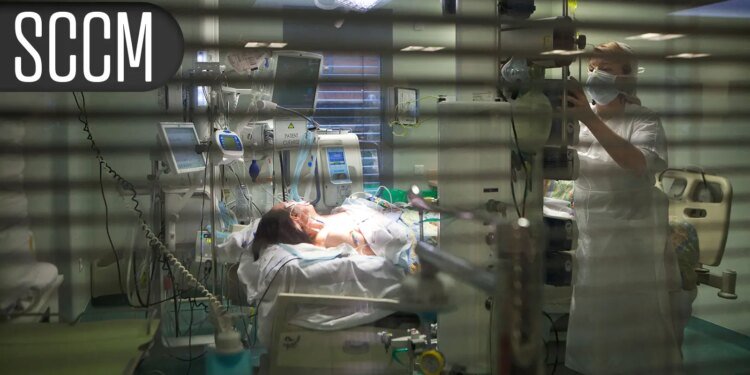
CHICAGO — Incorporating procalcitonin into an algorithm for sepsis diagnosis in the emergency department did not affect the timeliness of patients receiving IV antibiotics, but it did reduce short-term mortality rates, the randomized PRONTO study showed.
Among over 5,000 patients, 48.6% of those receiving procalcitonin-guided care were given IV antibiotics at 3 hours versus 48.2% of those receiving usual care (P=0.91), but 28-day mortality was significantly lower in the intervention group (13.6% vs 16.4%, P=0.0094), reported Stacy Todd, PhD, of Liverpool University Hospitals NHS Foundation Trust in England, at the Society of Critical Care Medicine annual meeting.
The study was also published in Lancet Respiratory Medicine.
“We hypothesize that there are multiple subtle changes to clinician behavior that haven’t been measured within the current process framework,” Todd told attendees.
“We see this improvement in mortality in both infection diagnosis and non-infection diagnosis, so changes are happening beyond just what we’ve seen in infection management,” she said. “One of our working hypotheses,” she added, is “that the same percentage of patients are getting antimicrobials, but the right patients are getting antimicrobials.”
The team is planning additional research “to understand the mechanisms behind this mortality reduction,” Todd noted, “accepting that this will be vital for clinicians to have confidence in any intervention such as this to be able to be implemented in patient care.”
Procalcitonin has been well established as a biomarker that rapidly responds to bacterial infection with high specificity, but previous trials assessing its utility in diagnostic algorithms for sepsis have been too heterogeneous or otherwise inadequately rigorous.
The ADAPT-Sepsis randomized trial of critically ill patients with suspected sepsis showed that daily assessment of procalcitonin, rather than standard care alone, led to significantly less time on antibiotics cumulatively in the first 28 days, while meeting noninferiority criteria for all-cause mortality.
Judi Jacobi, PharmD, a former critical care pharmacist at Indiana University Health in Lebanon, told MedPage Today that it’s “really impactful” to see this question studied on such a large scale.
“It’s an important study because we have thought that procalcitonin would be beneficial to our decision-making, but honestly, no one’s really been able to establish that it is,” Jacobi said.
“What surprised me is that it didn’t influence antimicrobial prescribing practices since we’ve made procalcitonin part of many of our antimicrobial stewardship programs for that express purpose,” she added. “Maybe their clinicians are just better at selecting patients for antimicrobials, or perhaps procalcitonin really doesn’t make a difference.”
After the presentation, she asked whether the Hawthorne effect might be playing a role in the mortality benefit, though that would not necessarily explain the similar rates of antibiotic use.
“I think it’s going to be really exciting to see what sort of hypotheses they can generate from that to figure out the reasons for the findings,” she said.
In an accompanying comment, Stephanie Cabral, MD, and Chanu Rhee, MD, MPH, of Harvard Medical School in Boston, suggested that “the most plausible mechanism is improved diagnostic clarity at an early and highly consequential decision point.”
“A high procalcitonin result might reinforce the diagnosis of bacterial sepsis and prompt earlier escalation of sepsis-directed care, whereas a low procalcitonin result might catalyze earlier consideration of alternative diagnoses and broader evaluation even if empirical antibiotics are still given,” they wrote.
From November 2020 to November 2023, Todd and colleagues enrolled 7,667 patients ages 16 and older who presented to any of 20 emergency departments across England and Wales with suspected sepsis. They excluded patients receiving end-of-life care or immunosuppressive chemotherapy, and those undergoing transplant or an urgent surgical intervention.
The final primary analysis included 2,715 patients assigned to usual care and 2,738 patients assigned to care guided by an algorithm incorporating procalcitonin labs, though clinicians could use or ignore those results. Across the two groups, median age was 72-73, 50-51% were women, and 85% were white. Characteristics were also similar between the two groups in symptom duration prior to enrollment, history of antibiotics in the 2 weeks before admission, comorbidities, and C-reactive protein levels.
Procalcitonin-guided care results were considered in clinical decision-making in 64.7% of cases, and the clinicians agreed with the algorithm’s recommendation in 47.2% of cases. Among 1,944 cases initially classified as high risk, consideration of procalcitonin labs reclassified 24.6% as low risk and 33% as medium risk.
Mortality was lower at 90 days in the procalcitonin-guided care group versus the usual care group (20% vs 23.8%, P=0.0018). “Time to death was also significantly different between groups,” the researchers wrote. “A significant interaction was estimated between deprivation decile and procalcitonin-guided care for mortality outcome, with the largest benefits in the most deprived groups.”
Planned subgroup, sensitivity, and secondary analyses did not explain the mortality benefit for procalcitonin-guided care. No other statistically significant treatment effects on other secondary outcomes were identified, including days on antibiotic treatment. Among 180 adverse events, 53.3% were in the usual care group and 46.7% were in the procalcitonin-guided care group.
Source link : https://www.medpagetoday.com/meetingcoverage/sccm/120481
Author :
Publish date : 2026-03-25 17:56:00
Copyright for syndicated content belongs to the linked Source.