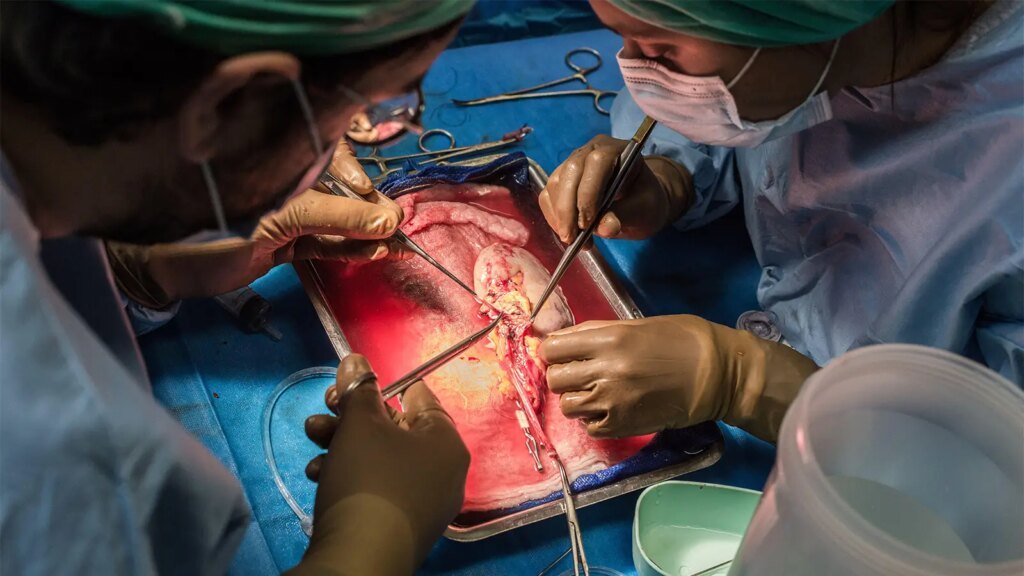
With no known cure for focal segmental glomerulosclerosis (FSGS), many affected patients opt for kidney transplant. But even after kidney transplant, FSGS can recur.
FSGS is a progressive kidney disease with an incidence of roughly seven to eight new cases per million people each year. It causes scarring in glomeruli that leads to nephrotic syndrome and eventual loss of kidney function.
Depending on the type of FSGS, patients can be managed with glucocorticoids or supportive therapy. However, over half of patients progress to kidney failure within 5 to 10 years after diagnosis and require dialysis or kidney transplant.
“Recurrence of FSGS after kidney transplantation significantly increases allograft loss, leading to morbidity and mortality,” said authors of a 2024 consensus statement.
Post-Transplant Recurrence Rates
FSGS recurs in 14-60% of first-time transplants and up to 80% of subsequent transplants, according to a 2022 review by Rachel Engen, MD, of the University of Wisconsin–Madison, and co-authors.
“Forty to sixty percent of these recurrences result in graft loss, and recurrence of FSGS was the cause of 3.2% of all graft failures in a North American Pediatric Renal Trials and Collaborative Studies report,” Engen and co-authors noted.
A 22-study meta-analysis of 966 patients identified several factors significantly tied to an increased risk of FSGS recurrence after transplant. These included:
- Proteinuria before kidney transplant (standardized mean difference [SMD] 2.04)
- Having a related donor (OR 1.99)
- Nephrectomy of native kidneys (OR 6.53)
- Age at transplantation (SMD -0.47)
- Age at onset (SMD -0.31)
- Time from diagnosis to kidney failure (SMD -0.24)
Factors not associated with post-transplant FSGS recurrence included human leukocyte antigen (HLA) mismatches, duration of dialysis before kidney transplant, sex, living donor, tacrolimus use, and previous transplantation.
A 2024 retrospective study compared the rate of new-onset and recurrent FSGS in kidney transplant patients. Within 65 months of transplant, five of 24 patients developed recurrent FSGS (estimated as incidence of 26.3%). Two of the five patients experienced graft failure. Nine of 749 patients without a history of FSGS developed it after transplant (incidence of 1.2%), three of whom had graft failure.
Compared with recurring FSGS, patients with new-onset FSGS had slower graft loss, yielding a higher graft survival rate (probability of graft survival 60% vs 33.3%, P=0.036).
Ways to Prevent Recurrence
Currently, there are no routinely recommended treatments to prevent FSGS recurrence after transplant, but the clinical course of FSGS before end-stage renal disease (ESRD) may offer insight into recurrence risk, Engen and co-authors wrote.
“For example, initial steroid responsiveness that evolves to secondary steroid resistance appear to have a higher risk of recurrent disease (78%-93%) compared with patients with initial steroid resistance (30%-39%), presumably because the latter were more likely to have a genetic cause of FSGS,” they noted.
Pre-transplant therapy with rituximab and plasmapheresis has been proposed to prevent recurrent FSGS after transplant, though supporting data are mixed. A small 2005 study reported eight rounds of preemptive plasmapheresis prevented recurrence in seven out of 10 patients, including three out of six who had previously lost a graft to recurrent FSGS.
However, a 2024 observational study of transplant recipients who already had an FSGS relapse on a previous graft found no difference in the time to progression to end-stage renal disease between those who received prophylactic treatment with IV cyclosporine, rituximab, or plasmapheresis or a combination thereof compared with no prophylaxis.
Renin-angiotensin-aldosterone system blockade with ACE inhibitors and angiotensin receptor blockers might also prevent FSGS recurrence by reducing protein excretion, though it is sometimes avoided after transplantation because of risk for decreased renal blood flow and hyperkalemia.
“The efficacy of current treatments, especially extracorporeal therapies and rituximab, requires large, prospective, randomized controlled trials, such as the ongoing PRI-VENT FSGS study to ensure that current common practices are providing the best results,” said Engen’s group.
They called for further research to test emerging and investigational therapies for pre-transplant FSGS in transplant recipients, including SGLT2 inhibitors, dual endothelin type A and angiotensin II type 1 receptor antagonists like sparsentan (Filspari), TNF inhibitors like adalimumab (Humira), TRPC5 channel inhibitors, and ROBO2/SLIT2 inhibitors.
Please enable JavaScript to view the comments powered by Disqus.
Source link : https://www.medpagetoday.com/spotlight/fsgs/121055
Author :
Publish date : 2026-05-01 13:43:00
Copyright for syndicated content belongs to the linked Source.