For decades, colorectal cancer prevention has been framed around a simple principle: find polyps early, remove them, and repeat colonoscopy to prevent cancer down the line. This approach has saved lives. But like many well‑intentioned practices in medicine, what works well at one stage of life may offer diminishing, and even negligible, returns at another.
Our study, recently published in JAMA, challenges a deeply ingrained assumption in gastrointestinal care that older adults with a history of precancerous polyps (known as adenomas) should routinely continue follow-up colonoscopies well into their late 70s and beyond. The data tell a more nuanced story, one that should prompt clinicians and health systems to reconsider how we balance cancer prevention against competing health risks in aging populations.
Why We Asked This Question
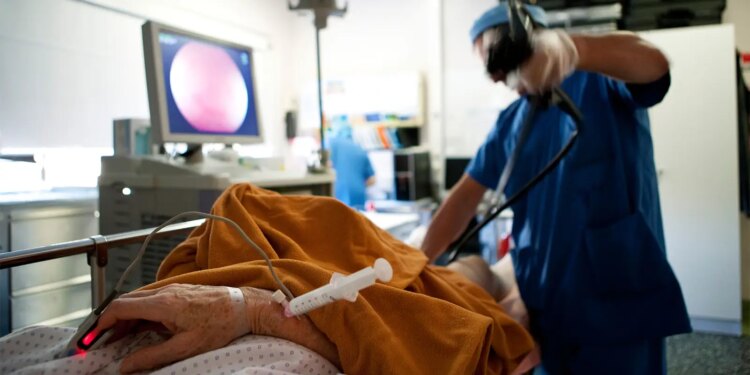
As gastroenterologists, we regularly face a difficult clinical dilemma. We know that precancerous polyps increase future colorectal cancer risk. We also know that progression from polyp to cancer typically takes many years, while the risks of colonoscopy — bleeding, perforation, cardiovascular events — increase with age. Yet follow-up colonoscopies (also referred to as surveillance colonoscopies) often continue by default, even when patients are older and living with multiple chronic conditions.
Our goal was straightforward: to estimate the actual risk of colorectal cancer and colorectal cancer-specific death after age 75 among people with prior adenomas; compare that risk with people who previously had a normal colonoscopy; and weigh both against the competing risk of dying from other causes. We hypothesized that among adults who remained cancer‑free until age 75, colorectal cancer risk would be low and dwarfed by non-colorectal cancer mortality. That hypothesis proved correct.
What We Studied and What We Found
Using national data from the Department of Veterans Affairs, we followed approximately 92,000 adults who underwent colonoscopy before age 75 and tracked outcomes for up to a decade. About 28% had adenomas detected on their earlier examination; 72% did not.
The results were striking in their simplicity. At 10 years of follow‑up among adults ages 75 and older, the cumulative incidence of colorectal cancer was just 1.1% in those with prior adenomas and 0.7% in those without. Colorectal cancer-specific death was even rarer: 0.5% and 0.4%, respectively. At 5 years, these risks were roughly half those values.
By contrast, the competing risk of death from causes other than colorectal cancer was substantial — about 22% at 5 years and nearly 50% at 10 years. In other words, regardless of prior adenoma status, older adults were overwhelmingly more likely to die from something other than colorectal cancer.
While people with prior polyps did have a relatively higher cancer risk than those without, the absolute risks were very low. Absolute risk, not relative risk, is what matters most when patients and clinicians are weighing whether another invasive procedure is likely to help.
Overall Health Changes the Equation
We also looked beyond age alone and examined outcomes based on people’s overall health, specifically their strength, medical complexity, and ability to recover from illness or procedures.
Among older adults with a history of adenomas, the chance of dying from causes other than colorectal cancer varied dramatically depending on overall health status. For those in relatively good health and able to function independently, about one‑third died from non-colorectal cancer causes over the next 10 years. For those with significant medical problems and limited physical resilience, that risk exceeded 80%.
Across every level of overall health, older adults were far more likely to die from heart disease, lung disease, infections, or other conditions than from colorectal cancer. Even among those with previous precancerous polyps, the risk of developing or dying from colon cancer remained very low compared with the risk posed by other health problems.
Age alone is an incomplete guide for deciding whether to have a follow-up colonoscopy.
Why Current Practice Falls Short
Guidelines already recommend against routine screening colonoscopy after age 75 for average‑risk adults. Follow-up colonoscopy after adenoma removal, however, often continues simply because a polyp was found years or decades earlier.
This persistence is understandable. Clinicians worry about missing a preventable cancer, fear litigation, and inherit longstanding practice habits. But colonoscopy is not a zero‑risk intervention, particularly in older adults with multimorbidity.
When the likelihood of benefit is exceptionally small, even modest procedural harms take on outsized importance. Our findings suggest that for many adults over 75, including those with a history of adenomas, the marginal benefit of follow-up colonoscopy is minimal when placed against their overall mortality risk.
Toward More Individualized Care
This study is not an argument to abandon colorectal cancer prevention in older adults. It is a call to modernize how we individualize it.
For many older adults, particularly those with moderate or severe frailty, it may be more appropriate to de‑prioritize surveillance colonoscopy in favor of interventions that more meaningfully improve longevity and quality of life: optimizing cardiovascular risk, managing diabetes, preventing falls, or addressing cognitive decline. For healthier, non‑frail older adults with substantial life expectancy, follow-up colonoscopy could be considered, but even adults in this category should know that their risk of developing or dying from colon cancer is incredibly low.
Crucially, this decision should not be made unilaterally. It belongs in a shared decision‑making conversation informed by absolute risk, competing health priorities, and patient values, and not by reflex or habit.
The goal is not to do more, or less, but to do what matters most for each patient. Evidence like this challenges us to rethink default practices and move toward care that is truly patient‑centered and value‑based.
Source link : https://www.medpagetoday.com/opinion/second-opinions/121021
Author :
Publish date : 2026-04-29 16:28:00
Copyright for syndicated content belongs to the linked Source.