- Guidelines recommend red blood cell exchange transfusion for selected patients with severe babesiosis, though this recommendation is backed by “low-quality evidence.”
- Red blood cell exchange transfusion reduced the risk of in-hospital death and 30-day readmission in a cohort of patients with severe babesiosis.
- Patients ages 70 and older and those with more severe organ damage may benefit most from red blood cell exchange transfusion.
Red blood cell exchange transfusion (ET) reduced the risk of in-hospital death and 30-day readmission in patients with severe cases of the tick-borne disease babesiosis, according to a target trial emulation using data from a multicenter cohort study.
Among 629 patients hospitalized with severe babesiosis, 3.6% of those treated with ET died or were rehospitalized within 30 days compared with 9.8% of those who didn’t undergo ET (adjusted OR 0.22, 95% CI 0.09-0.51), reported David Leaf, MD, of Brigham and Women’s Hospital in Boston, and his STOP-BABESIOSIS colleagues.
The ET treatment group also had a significantly greater average drop in parasitemia 1 day after treatment versus those who didn’t undergo ET (-59.7% vs -29.1%, respectively, P<0.001), they noted in JAMA Internal Medicine.
The findings have important implications, Leaf and colleagues wrote. “The magnitude of benefit — a nearly 5-fold reduction in the odds of the primary endpoint — suggests that ET should be strongly considered for patients meeting the eligibility criteria used in the present study.”
Patients were eligible if they had parasitemia greater than 10%, or 5% to 10% with either acute organ injury or severe hemolytic anemia.
“Future studies should further investigate which subgroups may benefit the most from ET, as well as its efficacy for patients with babesiosis who did not meet our strict eligibility criteria, such as those with milder degrees of acute organ injury,” the authors concluded.
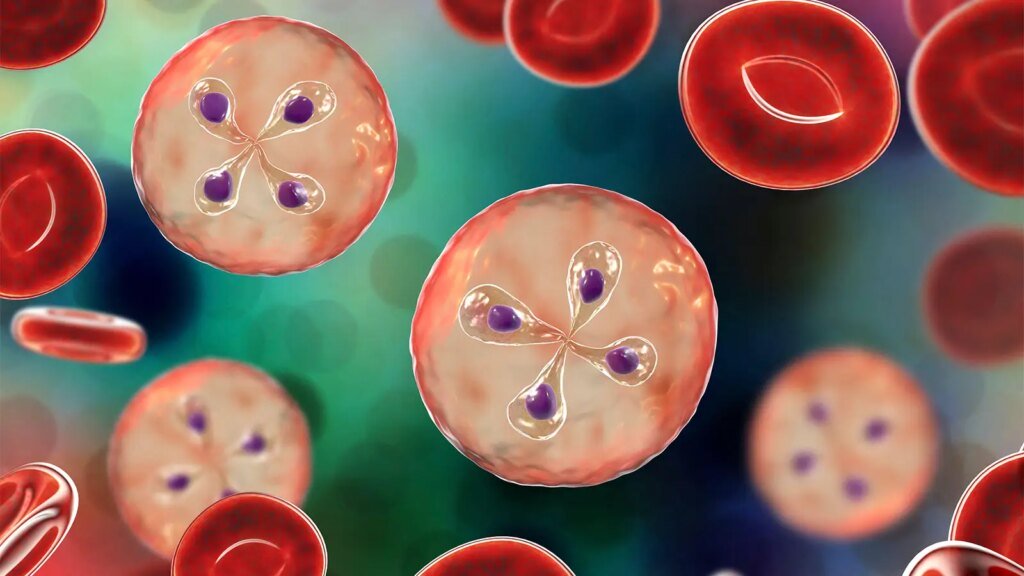
Babesiosis is a tick-borne disease caused by the parasite Babesia microti, which infects red blood cells. Symptoms include fever, chills, and headache, and clinical presentations range from asymptomatic infection to anemia, hospitalization, and death. At least 24 states have reported babesiosis cases, with 1,827 cases reported in 2020. The disease’s incidence is rising, particularly in the northeastern U.S.
ET removes infected red blood cells and transfuses donor red blood cells. The procedure is used as an adjunctive therapy to antiparasitic and antibiotic medications. Guidelines released in 2020 by the Infectious Diseases Society of America recommend ET for selected patients with severe babesiosis, but that recommendation is characterized as “weak” and backed by “low-quality evidence.”
The new findings on ET provide “the strongest clinical evidence to date supporting its targeted use despite long-standing uncertainty and limited prospective data,” noted Eric Meyerowitz, MD, and Johanna Daily, MD, both of the Albert Einstein College of Medicine in the Bronx, New York, in an accompanying commentary.
The study doesn’t resolve the clinically important question of which patients are most likely to benefit most from ET, they pointed out. Despite this, the findings “suggest that patients with high parasitemia, but minimal organ dysfunction, experienced limited benefit from ET, whereas older patients or those with SOFA [Sequential Organ Failure Assessment] scores greater than 12 receive the greatest benefit,” Meyerowitz and Daily wrote.
The study highlights the need for more research to shape babesiosis practice guidelines on when to start ET and when repeated ET sessions are necessary, they added.
This target trial emulation used data from a multicenter cohort study of 3,233 consecutive adults hospitalized with babesiosis from 2010 to 2024 at 82 sites across the northeastern U.S.
Leaf and colleagues included 629 patients (median age 71, 70.9% men), 33.2% of whom received ET in the first 7 days of hospitalization. Median parasitemia and immunocompromised status were greater among those in the ET group.
Those who received ET had lower adjusted risks of in-hospital death compared with those who didn’t (2.2% vs 2.9%), as well as lower risks of 30-day readmission (1.6% vs 7.1%). The ET group was also less likely to have persistent or progressive organ injury (9.2% vs 18.8%). Median hospital length of stay wasn’t significantly different between the two groups (7 days each). Among the ET group, 22% of patients had a second ET treatment, while 2.9% underwent a third treatment.
In the ET group, patients ages 70 and older had better primary endpoint outcomes versus those younger than 70, as did those with greater organ dysfunction, defined as SOFA scores greater than 12. Outcomes were also better in ET patients with parasitemia greater than 10% compared with those with parasitemia between 5% and 10%.
Study limitations included greater illness severity among patients who underwent ET. The total number of deaths among study participants was relatively low, which meant readmissions accounted for most of the composite endpoint’s events. The study included only patients hospitalized in the northeastern U.S., which may affect the findings’ generalizability.
Please enable JavaScript to view the comments powered by Disqus.
Source link : https://www.medpagetoday.com/infectiousdisease/generalinfectiousdisease/120631
Author :
Publish date : 2026-04-03 14:50:00
Copyright for syndicated content belongs to the linked Source.