Alpha-gal syndrome (AGS) is a severe tick-vectored food allergy caused by sensitivity to the galactose-alpha-1,3-galactose (alpha-gal) carbohydrate. It is now estimated to affect as many as 450,000 residents of the United States, yet it is not widely known.
Although AGS can be life-threatening, a 2022 survey found that 42% of healthcare practitioners had never heard of it and an additional 35% were “not too confident” in their ability to diagnose and manage the condition.
The diagnostic landscape, however, appears to be improving, according to a recent case-control study in JAMA Network Open.
The study looked at timely diagnosis as reported by patients at a North Carolina allergy clinic. The overall time between first symptom onset and confirmed AGS diagnosis has shortened 70-fold since 2009-2011. But disparities among different populations in access to timely diagnosis and care still persist.
Higher educational attainment was the only measured demographic factor associated with improved diagnosis time, reported a team led by Caroline K. Maki, MPH, an epidemiology researcher at the Rickettsial Zoonoses Branch, Centers for Disease Control and Prevention (CDC), Atlanta, but diagnosis took longer for those with less education.
Alpha-Gal Syndrome
The alpha-gal molecule, transferred by a bite from a tick, is found in mammalian meat, mammal-derived products, and pharmaceuticals. The distribution of AGS cases in the United States closely resembles that of the “lone star” tick, Amblyomma americanum, which is indigenous to the Eastern states.
“Alpha-gal cases have been increasing, particularly in regions with high tick populations like the southeastern United States,” allergist Ruchi S. Gupta, MD, MPH, professor of pediatrics and medicine at Northwestern Feinberg School of Medicine in Chicago, told Medscape Medical News. “However, awareness among clinicians is still growing, and underdiagnosis remains a concern.”
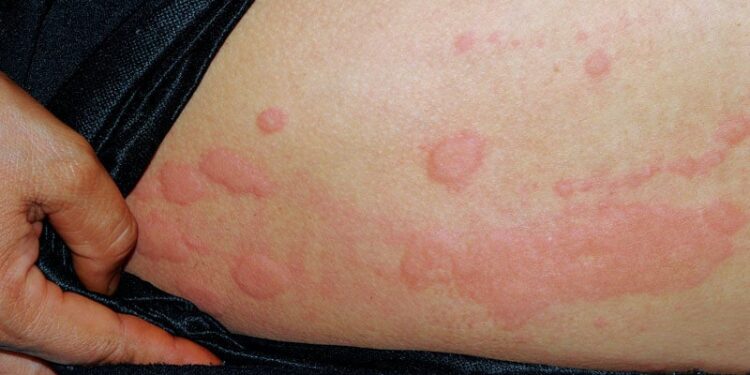
Symptoms of AGS, such as angioedema, urticaria, gastrointestinal distress, and delayed anaphylaxis, present 2-8 hours after exposure. “Although symptoms overlap with those of typical food allergies, a key difference is the delayed reaction, often 3-8 hours after eating red meat, making diagnosis more challenging,” Gupta added. “If a patient reports delayed allergic reactions, especially at night after eating red meat, consider alpha-gal.” Patients should be advised to avoid tick exposure and follow dietary restrictions. “Prescribe epinephrine and discuss new treatment options such as omalizumab [Xolair].”
Severity varies among individuals. “And the psychological impact is significant, as patients must drastically change their diets and lifestyles,” Gupta said, noting that research is ongoing, particularly on the duration of the allergy and potential desensitization approaches.
Lone star ticks are also linked to infections such as Rocky Mountain spotted fever and Southern tick–associated rash illness, but messaging about this pest has taken a back seat to that for the Lyme disease–associated black-legged tick.
The Study
Data were collected through a case-control study conducted jointly by the CDC and the University of North Carolina at Chapel Hill’s Allergy & Immunology Clinic. Of the 83 AGS patients from the clinic, 57 (69%) were residents of North Carolina, with 73 (88%) self-reporting as White race and 46 (55%) as women.
A comparison with a 2017 AGS cohort from the same allergy clinic looked at diagnosis trends over time.
For the quarter of patients (n = 18) with the earliest reported symptom onsets from 1977 to 2011 (analysis restricted to 2009-2011), the mean diagnosis time was 5.3 years (SD, 3.7). For the quarter of patients with the most recent symptom onsets, all in 2019 (n = 18), the mean diagnosis time was 28 days (SD, 24), a 70-fold improvement over that in the early group.
In addition, there was a 3-year mean difference in diagnosis time between the highest and lowest education groups: 1.4 years for those with graduate degrees and 4.4 years for those with high school diploma holders.
“The delay in diagnosis for those with lower levels of education highlights a clear gap in access to care, even among this unique cohort with eventual access to a medical specialist and AGS expert,” Maki and colleagues wrote. They stressed that healthcare practitioners should have “a well-rounded awareness of the factors that may influence patients’ abilities to receive timely AGS diagnoses to ensure the highest level of care and avoid undue physical, mental, and financial burden.”
The researchers acknowledged that the healthcare community is challenged to stay abreast of emerging illnesses through traditional medical literature channels. “Presently, patients more often discover a diagnosis of alpha-gal allergy by using information resources on their own than by presenting to the emergency department with anaphylaxis,” they wrote.
“Medical education is improving, but alpha-gal is still underrepresented in standard allergy training,” said Gupta. “Some regions are incorporating it more actively due to rising cases.”
She said primary care doctors and emergency department physicians should familiarize themselves with the signature delayed nature of alpha-gal reactions. “In addition, public health campaigns in tick-prone areas and clearer food labeling for mammalian products such as gelatin and dairy derivatives could help.”
The authors acknowledged the study was limited by not accounting for all disparities that may exist upstream of presenting to care. “Underscoring such disparities in AGS diagnoses should continue in more representative datasets,” they wrote. “As we learn more about the growing population of patients with AGS in the US, the disparities suggested by this study may become more apparent.”
This project was supported in part by an appointment to the Research Participation Program at the CDC administered by the Oak Ridge Institute for Science and Education through an interagency agreement between the US Department of Energy and the CDC. Maki had no competing interests. Co-authors Eleanor F. Saunders and Scott P. Commins reported receiving nonfinancial support from the American Academy of Allergy, Asthma, and Immunology outside the submitted work. Commins reported receiving grants from NIH-NIAID during the conduct of the study, personal fees from Genentech’s and Regeneron’s advisory board, and author royalties from UpToDate outside the submitted work.
Diana Swift is an independent medical journalist based in Toronto, Ontario, Canada.
Source link : https://www.medscape.com/viewarticle/novel-food-allergy-tick-borne-molecule-now-more-likely-be-2025a10005xd?src=rss
Author :
Publish date : 2025-03-11 12:46:00
Copyright for syndicated content belongs to the linked Source.