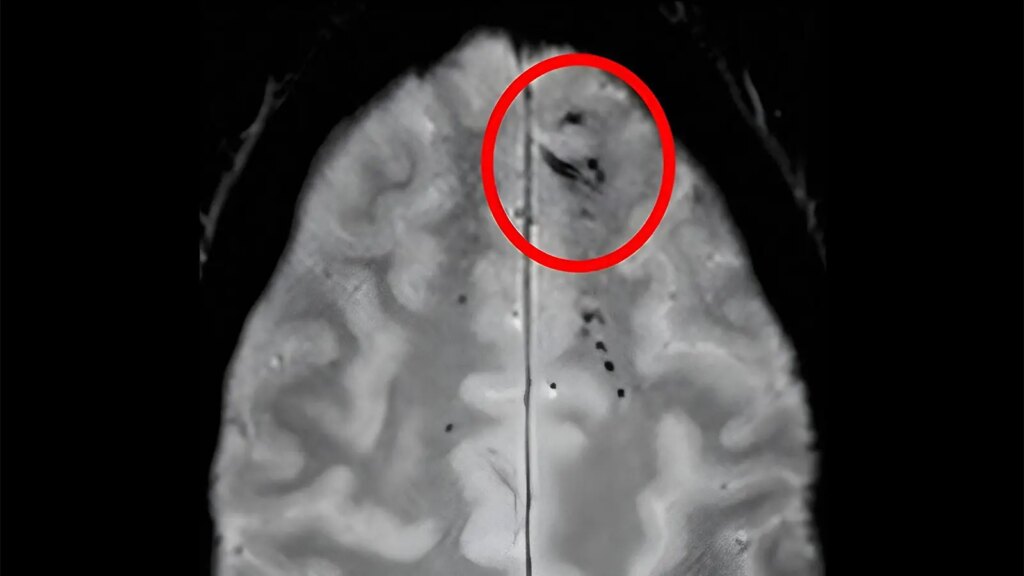
- In a cohort study, brain imaging results showing cerebral microbleeding had varying associations with dementia depending on the specific microbleed pattern.
- An increased risk of dementia was tied to microbleeds in lobar regions, lobar plus subcortical regions, or cortical superficial siderosis only.
- A larger number of microbleeds, regardless of location, was associated with a higher risk of dementia as well.
The location and amount of brain microbleeds that a person has could be telling of their risk of dementia, according to an observational analysis.
Compared with controls with no cerebral microbleeds detected on MRI, there was an increased dementia risk in older people with:
- Mixed subcortical and lobar microbleeds (HR 1.99, 95% CI 1.40-2.83)
- Lobar-only microbleeds, with or without cortical superficial siderosis (HR 1.96, 95% CI 1.30-2.97)
- Any cortical superficial siderosis (HR 2.57, 95% CI 1.36-4.89)
Participants with three or more cerebral microbleeds of any pattern also had an increased risk of dementia (HR 1.92, 95% CI 1.35-2.72), as did peers with at least two subcortical microbleeds, according to Rebecca Gottesman, MD, PhD, of the National Institute of Neurological Disorders and Stroke in Bethesda, Maryland, and colleagues.
Their report, based on the Atherosclerosis Risk in Communities-Neurocognitive Study, was published in Stroke.
“These findings show how different pathologies, represented by certain microbleed patterns, exhibit different associations with dementia development, but that severe enough pathology, represented by the frequency of microbleeds, increases dementia risk regardless of CMB [cerebral microbleed] cause,” the investigators concluded.
Cerebral microbleeds, the neuroimaging findings of small blood product deposits, can be considered a sign of cerebral small vessel disease and have previously been associated with dementia and subsequent stroke. Regarding specific microbleed patterns, prior work suggests that microbleeds in the lobar regions and cortical superficial siderosis are consistent with cerebral amyloid angiopathy (CAA), whereas subcortical microbleeds indicate a hypertensive cause.
For individuals with a lobar microbleed pattern, Gottesman’s group said, “a link between radiographic CAA and [Alzheimer disease] is possible, as both may reflect abnormal amyloid-β production and reduced clearance, albeit with deposition in distinct tissues.”
The authors argued that it is less likely that cerebral microbleeds themselves cause symptoms of dementia in people with mixed microbleed patterns and more microbleeds detected.
In those individuals, “it is more likely that the CMBs and their patterns of appearance reflect the underlying life-course exposure to vascular risk factors, such as hypertension, which impacts cerebral structure and function via visible (i.e., cerebral [small vessel disease] and stroke) and not always visible (e.g., alterations in blood-brain barrier or glymphatic function) mechanisms,” they wrote.
“Further studies of individuals with an especially high burden of CMBs or particularly those with mixed CMBs, in whom underlying pathology is less clear, should evaluate mechanisms contributing to cognitive impairment and dementia in association with these CMB patterns,” Gottesman and colleagues urged.
Their study was based on a community-based longitudinal cohort, first recruited in the 1980s, that got MRI scans at study visit 5 (2011-2013) and had no prior intracerebral hemorrhage or dementia.
Participants meeting study criteria came out to 1,583 older adults (mean age 76 years), of whom 22.8% had cerebral microbleeds detected on MRI.
A 24.7% incidence of cumulative dementia was seen over a median of 23.6 years of follow-up (up through 2020).
Gottesman and colleagues reported that a subcortical-only microbleed pattern did not have a significant association with dementia (HR 1.04, 95% CI 0.78-1.39).
Additionally, a sensitivity analysis excluding people with clinical stroke suggested that the association between cerebral microbleeds and dementia is not fully accounted for by clinical stroke.
Study authors acknowledged that beyond the observational nature of the study, limitations included not accounting for specific dementia etiologies and having small sample sizes for certain subgroups of cerebral microbleeds.
Please enable JavaScript to view the comments powered by Disqus.
Source link : https://www.medpagetoday.com/neurology/dementia/120086
Author :
Publish date : 2026-02-27 20:08:00
Copyright for syndicated content belongs to the linked Source.