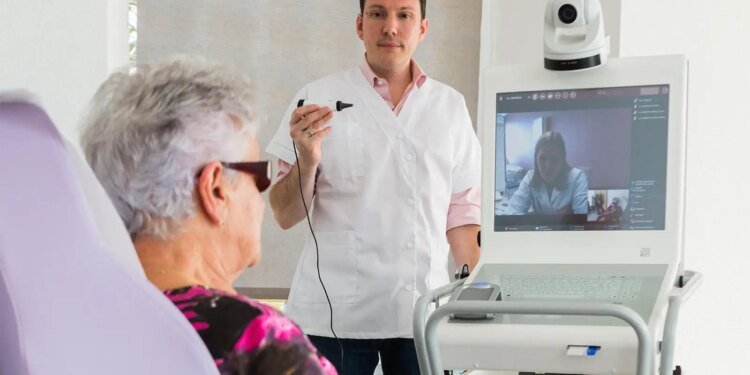
- A study compared telemedicine-guided versus conventional on-site subacute stroke care at over a dozen German hospitals with blinded expert assessment.
- Teleneurological ward rounds appeared to better meet care quality criteria set by guidelines, according to the observational analysis.
- These results support broader implementation of teleneurological ward rounds, though their effect on patient outcomes has yet to be studied rigorously.
Teleneurology ward rounds outperformed on-site consultations for patients in the subacute phase of stroke, a prospective study showed.
Across 15 hospitals within four German telestroke networks, complete adherence to six guideline-based quality domains — etiological classification, neurological examination, risk assessment, diagnostic recommendations, secondary prevention, and recommended aftercare — was achieved in 92% of cases during teleneurological ward rounds versus 54% of on-site ward rounds, reported Janina Behrens, MD, of Charité-Universitätsmedizin Berlin, and colleagues.
The study was designed as a noninferiority study but results met criteria for superiority, they noted in JAMA Neurology.
“The findings of this prospective multicenter study provide evidence that telemedicine-based neurological ward rounds in the postacute stroke unit setting achieve a high standard of quality care,” they authors wrote. “By ensuring guideline-adherent care and leveraging the expertise of network neurologists, teleneurological ward rounds can help close gaps in care quality and may improve long-term outcomes of stroke patients.”
Large-scale telestroke programs have already shown that teleneurological consultations are feasible in the U.S. and some European countries, though the focus has mostly been on stroke care in emergency departments, Behrens and team pointed out.
“However, the subacute phase of inpatient stroke care is equally important because it includes essential components of multifaceted stroke care, such as etiological diagnosis, risk stratification, prevention of complications, secondary prevention planning, and rehabilitation coordination,” they noted.
“To our knowledge, our study is the first that systematically compares the quality of teleneurological and on-site consultations in the postacute phase using blinded expert assessment,” they added. “The consistently better results of teleneurological assessments across all domains demonstrate that remote care can meet or even exceed the standards of traditional in-person care.”
In the VISIT STROKE study, each patient had two independent consultations on the telestroke unit within 3 days of hospital admission: one by network neurologists via video consultation, and the other by local neurologists on site. Documentation from both consultations was evaluated by blinded external experts.
Eligible adults had suspected acute ischemic or hemorrhagic stroke or transient ischemic attack and had undergone an initial neurological consultation on admission (either on site or via telemedicine) within 72 hours of symptom onset.
Out of 1,908 patients screened from 2022 to 2024, 518 were enrolled. Median age was 71 years, and 44% were women. Median NIH Stroke Scale score was 1.
Superiority of the virtual rounds was consistent across all quality domains, with the most pronounced advantage versus on-site ward rounds in guideline-adherent recommendations for secondary prevention (98% vs 77%).
“Teleneurological consultations are typically performed by experienced vascular neurologists within established networks, who are usually up-to-date with current guidelines and standardized protocols for stroke care,” Behrens and colleagues wrote. “In contrast, on-site assessments may be conducted by general neurologists or residents with varying grades of specialization and less routine use of structured assessment tools, potentially leading to less comprehensive evaluations.”
They nevertheless acknowledged that their study, on top of having an observational design, had the limitations of not assessing clinical outcomes and not enrolling patients with more severe neurological impairments.
“The value of in-person neurological presence for fostering team communication, education, and patient-centered interactions … should not be underestimated,” the authors cautioned. “Future research should include more severely affected patients and evaluate the impact of teleneurological ward rounds on patient-centered outcomes, cost-effectiveness, and healthcare team satisfaction.”
Source link : https://www.medpagetoday.com/cardiology/strokes/120666
Author :
Publish date : 2026-04-06 20:46:00
Copyright for syndicated content belongs to the linked Source.