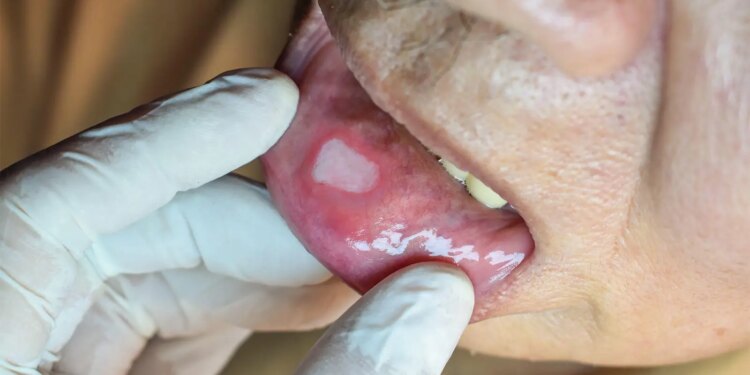
- Behçet’s syndrome is a form of autoimmune vasculitis marked by widespread and sometimes life-threatening cardiovascular complications, as well as skin, nervous system, and gastrointestinal lesions.
- Treatment has long relied on corticosteroids and immunosuppressant drugs such as methotrexate, but targeted biologic agents have recently joined the armamentarium.
- This updated guideline summarizes developments since the last version was released in 2018, with new evidence to support drug choices and withdrawal strategies.
Behçet’s syndrome poses some of the most difficult management challenges in all of rheumatology, but a newly updated guideline from the European Alliance of Associations for Rheumatology (EULAR) should help clinicians stay on top of the complexities.
The new guideline, developed by Gulen Hatemi, MD, of Istanbul University, and colleagues, comes 6 years after EULAR’s last edition released in 2018. Since that time, the authors observed, more evidence has emerged on which treatment regimens are best for certain clinical situations, with recent clinical trials comparing biologic and other targeted agents with old-line immunosuppressives and glucocorticoids.
A form of vasculitis, Behçet’s syndrome is a relapsing-remitting condition marked by potentially life-threatening cardiovascular complications, including thrombosis and aneurysms, as well as skin, eye, nervous system, and gastrointestinal involvement. Treatment is typically multifarious and is directed at patients’ particular manifestations, which may vary from one individual to the next. Behçet’s is sometimes called the “Silk Road disease” because its prevalence is especially high along the ancient overland trade route through Central Asia, connecting China with what is now Turkey.
Hatemi’s panel came up with 12 major recommendations covering mucocutaneous, vascular, joint, ocular, gastrointestinal, and parenchymal manifestations. For the most part, immunomodulatory drugs serve as the mainstays of treatment, even in patients with thrombosis for whom anticoagulants might be considered. The group noted that the most important change from the 2018 guidance is that more emphasis is now placed on tumor necrosis factor (TNF) inhibitors for managing many types of symptoms, both for inducing remission and for maintenance.
For patients with recurrent skin and/or mucosal lesions, “colchicine should be the first-line treatment,” the panel recommended, with TNF inhibitors or the phosphodiesterase-4 inhibitor apremilast (Otezla) for patients unresponsive or unable to tolerate the older drug. Skin ulcers can be treated with topical steroids, but “chronic use of systemic glucocorticoids should be avoided.”
Colchicine is also the top choice for joint manifestations, with immunosuppressants as second line.
Behçet’s patients with uveitis should definitely receive immunosuppressants, but never steroids as monotherapy, the committee concluded. TNF inhibitors, especially infliximab (Remicade), is called for when patients experience severe inflammation in the posterior segment.
High-dose steroids and infliximab should be the backbone of treatment for patients developing pulmonary or peripheral artery aneurysms. Steroids should not be given indefinitely, however; they should be tapered with TNF inhibitors serving as maintenance therapy. In cases requiring surgical intervention, this should proceed without delay. The panel recommended embolization over open surgery for pulmonary aneurysms at high risk for rupture.
Venous thrombosis should get basically the same drug regimen used for arterial complications, although anticoagulants may be added if patients appear at low risk for bleeding and have no pulmonary aneurysms. Surgery should be considered for patients with cerebral venous thrombosis.
For patients with gastrointestinal symptoms, Hatemi and colleagues recommended that management start with endoscopy. Drug therapies may include those commonly used for inflammatory bowel disease such as azathioprine, “with or without glucocorticoids,” and TNF inhibitors can be given in severe or refractory cases.
Finally, patients with any manifestations jeopardizing major organ functions should get high-dose steroids and infliximab or another targeted autoimmune drug. Again, steroids should be tapered once control is established and patients may then continue on targeted therapies for maintenance.
Most of the recommendations came with so-called Oxford evidence grades of 2, 3, and 5, indicating a foundation of cohort studies, case-control analyses, and expert opinion, respectively; a few were graded at 4, with case series as the basis.
“An important challenge when developing these recommendations,” Hatemi and colleagues noted, “was the heterogeneity of the trial populations and outcome measures that made it impossible to bring together the results in a meta-analysis or make comparisons between different therapeutic modalities.”
In consequence, the group suggested a research agenda to firm up the evidence base and inform the guideline’s next iteration. Much of it centered on randomized controlled trials to assess, for example, efficacy of newer biologic and targeted synthetic drugs both overall and for specific symptom categories. Optimizing doses and duration should be another research focus, along with identifying biomarkers for diagnosis and monitoring.
Other topics to address include the risks and benefits of various drug combinations, clearer definitions of key outcomes, and methods for determining how much continued disease activity (especially for skin and genital ulcers) patients can tolerate without needing more aggressive drug therapy.
Source link : https://www.medpagetoday.com/rheumatology/generalrheumatology/120466
Author :
Publish date : 2026-03-24 19:12:00
Copyright for syndicated content belongs to the linked Source.