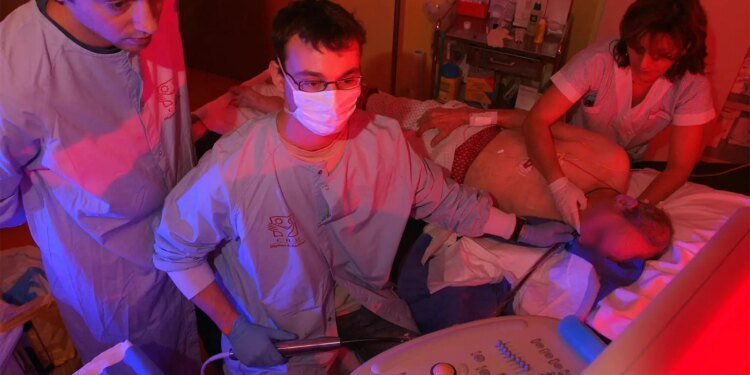
- A Taiwanese trial compared transesophageal echocardiography (TEE)-guided CPR with conventional chest compressions in patients with out-of-hospital cardiac arrest.
- It was expected that TEE would enable operators to avoid compressing the aortic valve for more direct compression over the left ventricle.
- The small trial was ultimately not able to show that TEE-guided CPR improved return of spontaneous circulation through enhanced hemodynamic effects.
The concept of transesophageal echocardiography (TEE) guidance during CPR hit a wall when tested for the first time in a randomized trial.
For patients who were in a prolonged out-of-hospital cardiac arrest (OHCA) and very sick upon arrival to an emergency department (ED), subsequent performance of TEE-guided CPR with compression site adjustment was no better than standard CPR.
There was no significant improvement in the patient’s likelihood of a sustained return of spontaneous circulation (ROSC) of at least 20 minutes (44% vs 39%; cluster-adjusted OR 1.21, 95% CI 0.64-2.29), nor secondary outcomes such as any ROSC (≥1 minute), survival to intensive care unit admission, survival to hospital discharge, and discharge with favorable neurological outcome, according to Jen-Tang Sun, MD, MSc, of Far Eastern Memorial Hospital in New Taipei City, Taiwan, and colleagues.
Nevertheless, TEE guidance was associated with a hemodynamic benefit of higher intra-CPR end-tidal carbon dioxide levels at minutes 11-20 after ED arrival. Moreover, there was no increase in adverse events, the EXECT-CPR study authors reported in JAMA Internal Medicine.
The premise of the TEE approach rests on the assumption that the ultrasound helps target chest compressions toward the left ventricle while avoiding the aortic valve; aortic valve compression has been associated with poorer prognosis and reduced diastolic and mean arterial pressures during CPR. TEE enables identification of the area of maximal compression without interrupting chest compressions.
The researchers said the 132-person EXECT-CPR trial was ultimately underpowered to show a benefit to TEE-guided CPR.
Notably, it may also not have been targeted to the right setting. “A key explanatory factor for the discrepancy between the observed hemodynamic benefit and the absence of survival improvement in our trial is likely the late timing of the intervention … patients had already undergone approximately 30 minutes of prehospital CPR, such that by 20 minutes in the ED, more than 50 minutes had elapsed since collapse.”
“At this stage, patients with favorable physiology may already have achieved ROSC, leaving a refractory cohort less responsive to further hemodynamic augmentation,” Sun and colleagues wrote, noting that their study group had a very low 4% survival rate and zero favorable neurological outcomes.
“Consequently, TEE-guided CPR may be more suitable for in-hospital cardiac arrest. For OHCA, a more effective strategy may be to integrate TEE into the prehospital setting to allow TEE-guided CPR as early as possible after collapse. Further research is needed to explore the feasibility and clinical impact of these two scenarios,” they concluded.
Editorialists led by Teva Brender, MD, of University of California San Francisco, shared the sentiment that TEE-guided CPR may not be for OHCA.
“Perhaps one of the most important takeaways is that TEE-guided CPR may be most appropriate in the inpatient setting (where trained operators and specialized equipment are already available) to improve outcomes for in-hospital cardiac arrest,” Brender and colleagues wrote in an accompanying editorial.
Even if this TEE approach did work out in an OHCA trial, they suggested, implementation would face considerable financial and logistical barriers. It would also depend on local training, licensing, and certification requirements whether TEE is within the relevant emergency responder’s scope of practice, they added.
In any case, much larger study samples would be needed in future investigation of TEE-guided CPR, according to the editorialists.
EXECT-CPR was a cluster-randomized clinical trial conducted in 2023 at one Taiwanese center. The study design consisted of a randomized sequence of 2-week scheduling blocks with trained TEE operators on standby during their assigned periods.
Overall, the study included 132 consecutive patients (median 68 years, 66% men) transported to the ED with ongoing, nontraumatic OHCA. Exclusion criteria were prehospital ROSC, extracorporeal CPR, contraindications to TEE, prior do-not-resuscitate orders, and obvious signs of death.
All patients had chest compressions initiated manually and transitioned to mechanical CPR for transport. Mechanical CPR continued in the ED unless it was not feasible there, and manual compressions were given instead.
In the TEE-guided group, TEE was performed after intubation to guide compression-site adjustment. In the conventional group, compressions were directed to the lower half of the sternum, with repositioning performed if displacement occurred. Resuscitation was terminated if ROSC was not achieved within 1 hour.
In the TEE-guided group, 59 out of 66 did get successful TEE imaging. Of the 36 patients who required adjustment, 92% had successful relocation that required a median of three repositionings over a median 23 seconds, completed at a median 8.5 minutes from ED arrival.
“While the study focused exclusively on using TEE to guide compression location, additional benefits, such as aiding in the diagnosis of aortic dissection, pericardial effusion, or other potentially reversible causes of arrest, might be considered in the overall decision to incorporate TEE into resuscitation,” Brender and colleagues commented.
“Future research will help clarify the utility, feasibility, and safety of TEE-guided CPR, including which settings and patient populations have a sufficiently high likelihood of functional recovery to justify the addition of this resource-intensive intervention,” according to the editorialists.
Source link : https://www.medpagetoday.com/emergencymedicine/emergencymedicine/120449
Author :
Publish date : 2026-03-23 20:02:00
Copyright for syndicated content belongs to the linked Source.