“The rats are coming, the rats are coming…” my writer friend Liz said last month as I considered titles for this column about a rat-borne parasite now in my home state of California. Said parasite recently led to the death of an animal at the San Diego Zoo.
“Well, not exactly,” I replied. “Some rats are already here.” Then I suggested “Rats Without Borders,” but Liz found it demeaning. Of course she was right. Connecting rats and global humanitarian heroes would not be good.
In the end, the title wrote itself. But first some backstory.
A Personal Parasite Saga
As a kid, I never had a pet rat, nor did I see many wild rats until I spent 3 months in Taiwan in 1983. No surprise there. As most people know, tropical islands are havens for the clever, long-tailed creatures.
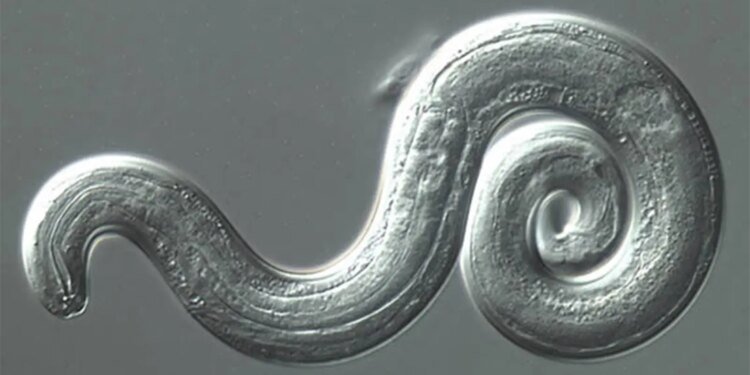
But 1983 marked another personal milestone: meeting my first-ever patient with rat lungworm disease (RLWD). When the 5-year-old was admitted to the hospital, her spinal fluid teemed with eosinophils, a finding highly suggestive of rat lungworm meningitis. It also contained live, coiled larvae of Angiostrongylus cantonensis, the formal name for the brain-invading parasite native to Asia. However, by the time her pediatrician brought me to her house a week or two later and she and I met in person, a hefty course of steroids had already helped her — so much so, in fact, that the recovered sufferer happily walked me down her lane to show me her family’s huge, steel-gray pig.
The girl had fallen ill at a time when people in Pingtung County still ate giant land snails braised in a flavorful sauce — a dish I myself sampled with colleagues who made darned sure the snail-meat was well-cooked. And for good reason. If not, we too might have ingested viable larvae of A. cantonensis that could later invade our central nervous systems.
In short, in humans, RLWD (also called neuroangiostrongyliasis) is both a food-borne and neurologic blight with mild, moderate, or severe (and occasionally fatal) sequelae. The infection starts when people consume raw or under-cooked gastropods that have previously dined on poop from A. cantonensis-infected rats. Or they eat “paratenic hosts” that have eaten other A. cantonensis-infected animals. Yet another source in humans is poorly-washed produce inhabited by (or possibly coated with slime released by) snails or slugs containing rat lungworm larvae.
Nonetheless, after 1983, I didn’t track the parasite’s spread until almost two decades later, when A. cantonensis sickened 12 of 23 medical students from Chicago who visited Jamaica during spring break. An investigation later published in the New England Journal of Medicine confirmed that the afflicted students ate a large, shared Caesar salad during the group’s final dinner.
That’s when I realized that A. cantonensis was not only present in most of Asia and the Pacific basin, including Hawaii (a major epicenter), but also, it had entered Jamaica and other Caribbean islands; countries in Africa such as Madagascar, Egypt and Nigeria; and certain continental U.S. states that now include Louisiana, Florida, Georgia, Oklahoma, and Texas, among others. Over the last decade, the parasite has also appeared in animal or human hosts from Brazil to the Canary and Balearic islands to coastal Italy and Spain.
Of course, it’s anyone’s guess if other eco-friendly ports also harbor A. cantonensis because no one has actually looked.
A Sad Event at the San Diego Zoo
This brings us to the parma wallaby — the world’s smallest member of the kangaroo family — euthanized in San Diego in December 2024 and described in a recently published CDC report.
After the wallaby suffered more than a week of head-shaking, abnormal movements, blindness, and paralysis, its necropsy revealed multiple bleeds in its brain and “half a dozen” A. cantonensis roundworms on membranes covering its cerebellum, brain stem, and spinal cord.
Researchers then identified A. cantonensis in two free-roaming rats at the zoo and seven staggering, brain-injured opossums rescued by animal lovers in various parts of San Diego County — which meant that infective larvae also lurked in nearby snails and slugs, and that a curious toddler or puppy who ate or played with one of them might be the next innocent bystander to suffer grave neurologic harm.
Thus, San Diego residents and tourists have now joined the list of people in the U.S. and beyond who need to make sure that:
- They only eat thoroughly-washed, fresh local greens;
- Responsible individuals keep a watchful eye on roving toddlers; and
- Children are warned to avoid contact with snails and slugs.
California doctors also need to familiarize themselves with RLWD’s early, variable symptoms and diagnose it (or, in the case of a likely exposure, sometimes empirically treat it) as early as possible. Today, prospective treatment frequently involves an anti-helminthic drug like albendazole (Albenza), although steroids are equally essential when clinical findings or diagnostic tests suggest that larvae are actively migrating or have already breached the central nervous system.
“With a Little Help from My Friends”
It goes without saying that RLWD is rare compared to many other tropical infections. Nonetheless, since it is now widely emerging due to globalization, climate change, and evolving human behaviors, public awareness is key. Accordingly, in 2019, my husband and I decided to underwrite an educational documentary. Three years later, “Accidental Host — The Story of Rat Lungworm Disease” began airing on PBS stations around the country. Today, it is streaming on PBS Hawai’i‘s YouTube channel.
Much of the credit for the final product belongs to patients and families who shared their stories along with terrific experts and filmmakers. But I need to mention two people in particular.
Thanks to Larry Ash, PhD, a renowned UCLA parasitologist who first studied A. cantonensis in the 1960s in French Polynesia and Hawaii, we gained a one-of-a-kind perspective on the parasite’s discovery, transmission, and spread. I only wish Ash were alive today to advise on next-steps in California. And Vernon Ansdell, MD, who I originally met while studying tropical medicine in London, later moved to Hawaii and became a principal advisor to the Hawaii Governor’s Task Force on Rat Lungworm Disease. His clinical insights and contacts proved essential to the making of our film.
And here’s a final piece of breaking news. This month, Ansdell and others published a paper about an outbreak of neuroangiostrongyliasis in six men in Hawaii linked to a novel exposure: drinking kava from a communal vessel in which a drowned slug was later found. The report is noteworthy because it underscores that treating early with albendazole has real clinical benefits, while it also ups concerns about A. cantonensis‘s potential for water-borne transmission — yet another reason for frontline doctors who see people at risk to keep rat lungworm on their radar. And, to state the obvious, another reason for residents and tourists in areas where A. cantonensis lives to avoid drinking untreated catchment water and to fight the urge to slake their thirst with water from a hose.
Source link : https://www.medpagetoday.com/opinion/parasites-and-plagues/120835
Author :
Publish date : 2026-04-18 16:00:00
Copyright for syndicated content belongs to the linked Source.