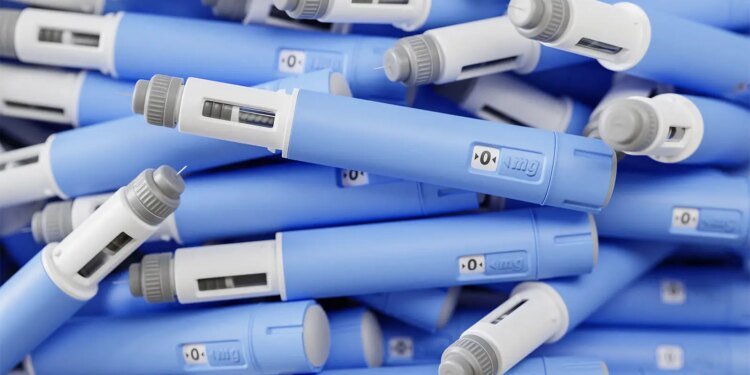
As a primary care physician and obesity board-certified specialist, I believe that GLP-1s are one of the best medical interventions of all time, right up there with vaccines, antibiotics, blood thinners, and statins. They really are revolutionary when it comes to treating obesity.
But what is “obesity”? Simply put, it is defined by CDC as a body mass index (BMI) ≥ 30 in adults. But medically this means very little, particularly because, in a heterogeneous society like America, we cannot have a singular definition. For example, according to the World Health Organization (WHO) and Asian-specific country medical guidelines, obesity among Asians is defined as a BMI equal to or over 25.
I raise this to emphasize two key issues: first, that physicians shouldn’t be using BMI to decide whether to prescribe a patient a GLP-1 drug — determination of a metabolic syndrome should be the driving factor — and second, to draw attention to the question of who should be taking GLP-1s versus who actually is taking them.
GLP-1s Go Mainstream
The FDA generally requires that clinical trials for weight loss drugs, like GLP-1s, show 5% or more weight loss compared to placebo in patients with BMI ≥ 30, or BMI ≥ 27 who also have one comorbidity. The clinical trial also must show improvement in at least one comorbidity. Under these criteria, the drugs are more likely to be approved and, in theory, covered by insurance.
Unfortunately, commercial insurance coverage has become more restrictive in the last few years given the high cost of these drugs. Because of this, many pharmaceutical companies have lowered their direct-to-consumer cash pay prices. Instead of thousands of dollars per month, it is often in the hundreds when patients pay out of pocket. Meanwhile, there are compounding pharmacies that make and sell their own version of GLP-1s that are not FDA-approved — but often come in at an even lower price point.
The price dip has allowed millions more Americans to access these drugs for weight loss. But the relevant medical question is, who actually needs a GLP-1?
Are the “Right” Patients Taking GLP-1s?
When I see a patient, in lieu of BMI I am searching for signs of metabolic syndrome or insulin resistance, which is a better way of describing “obesity.” Insulin resistance presents with some of the following signs and comorbidities: increased waist circumference (> 35 inches for women and > 40 inches for men), pre-diabetes or type II diabetes, fatty liver, obstructive sleep apnea, elevated triglycerides, and polycystic ovary syndrome, to name a few. These are often the patients (regardless of BMI) that can reap the greatest health benefit from GLP-1s.
GLP-1s are meant to be lifelong, as “obesity” is a chronic relapsing disease and insulin resistance worsens with time unless we intervene. Most of my patients with a metabolic syndrome have tried calorie restriction and exercise programs without sustainable results. Taking a medication to treat metabolic syndrome is not “cheating” (a term I hear often in society when people judge others’ weight loss journeys).
What does concern me is the person taking a GLP-1 to lose 10-to-20 pounds for casual weight loss. In December, the FDA approved the first oral GLP-1 pill for weight loss. It is now available at what appears to be the lowest price point to date, enabling more people to afford the drug. And just this week, FDA approved another drugmaker’s oral GLP-1 pill.
As people see their coworkers, family members, and celebrities going from plus-size to fat-free versions, everybody wants to jump on the bandwagon. Everyone seems so desperate to be thin. But at what cost?
We still don’t know the long-term impacts of GLP-1 use, and concerns have been raised about the potential for nutritional deficiencies and muscle loss. Furthermore, studies have shown that when GLP-1s are stopped, most if not all weight is regained within 1-2 years. I question whether the potential risks are worth the purely cosmetic benefits in otherwise healthy populations.
Meanwhile, there’s an underuse of GLP-1s in the population who can benefit most. Often, the very patients who stand to reap the most cardiovascular benefits and weight loss are the same patients who struggle most to afford them.
I don’t prescribe GLP-1s to patients without metabolic syndrome. A patient’s BMI is not really relevant to me, but it is for insurance coverage, which, as physicians know, is the greatest limiting factor to practicing medicine in this country.
My hope is that Medicaid and more private insurers opt in to cover weight-loss drugs for a broader swath of patients who need these drugs for health reasons. I also hope we change the definition of “obesity” to really identify patients who have metabolic syndrome and treat their disease appropriately. If people without metabolic syndrome want a piece of the pie (ahem, I mean protein shake), they can take a GLP-1 at their own risk.
Nidhi Kansal, MD, is a board-certified internal medicine and obesity medicine physician at Northwestern Medicine in Chicago.
Source link : https://www.medpagetoday.com/opinion/second-opinions/120612
Author :
Publish date : 2026-04-02 15:55:00
Copyright for syndicated content belongs to the linked Source.