- About a quarter of survey respondents who met USPSTF eligibility criteria were up to date with lung cancer screening in 2024 — an increase in prevalence of 6 percentage points since 2022.
- Lung cancer screening rates were low compared with those for other cancers, including colorectal, cervical, and breast cancers.
- Up-to-date prevalence was uneven depending on age, race and ethnicity, and insurance status.
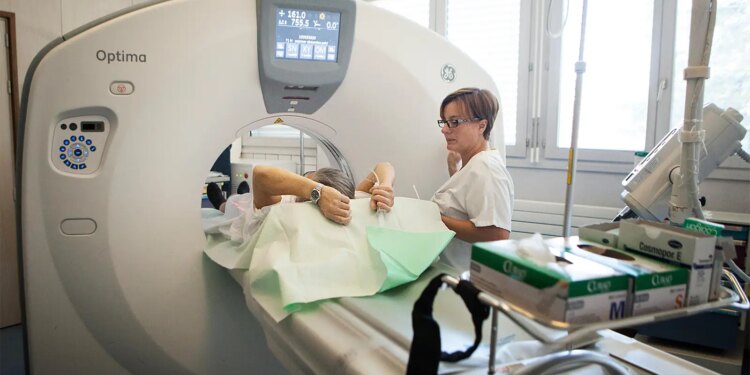
Lung cancer screening uptake with low-dose CT increased from 2022 to 2024, but remains low, according to a cross-sectional study.
Across the U.S., 24.49% of survey respondents who met U.S. Preventive Services Task Force (USPSTF) eligibility criteria were up to date on their lung cancer screening in 2024 — an increase in prevalence of 6 percentage points since 2022, with significant increases across most subgroups and no declines, reported Todd Burus, PhD, of the University of Kentucky in Lexington, and colleagues.
However, despite this improvement, “adherence to annual lung cancer screening remained low and uneven in 2024, underscoring the need to strengthen and expand programs and policies that increase uptake among eligible adults,” they wrote in a research letter in JAMA Internal Medicine.
In an accompanying editor’s note, Teva D. Brender, MD, of the University of California San Francisco, and colleagues noted that while the percentage of respondents up to date with screening “represents steady progress” compared with 2019 and 2022, screening rates “still lag far behind those for other recommended cancer screenings: 67.4% for colorectal, 75.4% for cervical, and 80.0% for breast cancer.”
They pointed out that research shows that lung cancer screening is less common among current smokers compared with those who have quit — “underscoring the need to incorporate both smoking cessation and [lung cancer screening] into cancer prevention strategies.”
“A decade after the first USPSTF recommendation for [lung cancer screening], we have welcome evidence of measured progress,” Brender and colleagues concluded. “However, work remains to better understand and address the structural barriers precluding eligible, high-risk individuals who would benefit from accomplishing this potentially life-saving intervention.”
For this study, Burus and colleagues used data from the 2024 Behavioral Risk Factor Surveillance System (BRFSS) national dataset — a population-based, state-representative survey of health behaviors — to calculate screening prevalence in 2024 (a self-report of CT to “scan or check for lung cancer” within the past year) among eligible individuals ages 50 to 80 years who were current smokers or quit within 15 years and had a smoking history of 20 or more pack-years.
The study sample included 26,104 respondents who met USPSTF eligibility criteria, representing 12.3% of U.S. adults ages 50 to 80 years. Of the eligible respondents, 54.4% were men, 78% were white, 7.3% were Black, and 6.5% were Hispanic.
Up-to-date prevalence increased with age — from 11.32% among those ages 50-54 to 31.20% among those ages 75-79. Compared with individuals with private insurance, up-to-date prevalence was significantly higher among those with military-related coverage (adjusted prevalence ratio [aPR] 1.83, 95% CI 1.52-2.20), Medicare (aPR 1.28, 95% CI 1.12-1.45), and Medicaid (aPR 1.23, 95% CI 1.04-1.46), and significantly lower among those without insurance (aPR 0.37, 95% CI 0.21-0.64).
The authors also found significant gains in many subgroups. For example, up-to-date prevalence increased by 4.52 percentage points among adults ages 50-54 (those who were first made eligible for screening in 2021), and by 15.69 percentage points among individuals with military-related insurance.
However, improvements were uneven, with no changes among Hispanic, Asian, or Black adults. “Culturally tailored outreach through community health workers and patient navigation may help increase screening uptake in these groups,” Burus and team wrote.
Brender and colleagues noted that “these findings suggest that payer policies, health system integration (i.e., Indian Health Service, Veterans Health Administration), and overall barriers to care associated with race can affect screening uptake.”
State-level up-to-date prevalence in 2024 ranged from 13.43% in South Dakota to 38.36% in Massachusetts, with the highest prevalences in the Northeast region. Twenty-one states had significant increases since 2022, spread evenly across regions. No states had significant declines.
Study limitations included biases inherent in self-reported data and the exclusion of 80-year-olds in temporal analysis.
Source link : https://www.medpagetoday.com/pulmonology/lungcancer/121007
Author :
Publish date : 2026-04-28 20:57:00
Copyright for syndicated content belongs to the linked Source.