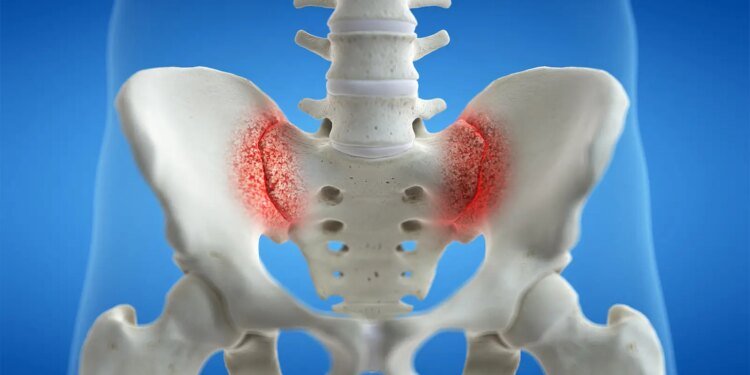
- MRI-detected sacroiliac bone marrow edema is a key diagnostic marker for axial spondyloarthritis (axSpA), but its value in ruling out other causes of patients’ symptoms depends on how common it may be in non-axSpA conditions, and its general prevalence is not well known.
- This study drew on data from a large, population-based German cohort who prospectively had whole-body MRI scans.
- Nearly 30% of this cohort showed sacroiliac bone marrow edema, with higher rates among women, overweight individuals, older men, and men who engaged in intense recreational physical activity — raising questions about axSpA diagnostic criteria.
Some 30% of a large general-population sample in Germany showed sacroiliac bone marrow edema (SBME) in MRI scans, a new study found, casting doubt on whether such findings are indicative of axial spondyloarthritis (axSpA).
Among members of the German National Cohort who underwent whole-body MRI scans from 2014 to 2016, SBME was found in 28.9% when images were read by human experts, and in 30.8% of a larger number of images analyzed by an artificial intelligence (AI) algorithm, according to Keno Bressem, MD, of the Technical University of Munich, and colleagues.
SBME rates were even higher in a number of subgroups: women in general, women who had been pregnant at some point, older men, men who engaged in intense recreational physical activity, people who were overweight, and those with physically demanding jobs, the researchers reported in Lancet Rheumatology.
These findings matter because MRI-detected SBME is a critical diagnostic marker for axSpA as enshrined in criteria set by the Assessment of SpondyloArthritis International Society (ASAS), which calls its presence “sufficient evidence of sacroiliitis,” Bressem and colleagues explained, especially early in the disease when joint inflammation isn’t visible on standard x-rays.
Diagnosing axSpA has traditionally been problematic because its early symptoms, i.e., lower back pain, can come from any number of things. Diagnosis was therefore a question of exclusion. With SBME seemingly a clear, objective, and specific marker for axSpA, the rheumatologist’s job was made a lot easier.
Now, with such a large proportion of people showing SBME without other indicators of axSpA, it’s no longer clear how much value it provides in ruling out other causes of patients’ symptoms.
“These population-based data provide essential reference values for accurate MRI interpretation and support the development of refined diagnostic and classification approaches that integrate patient demographics, bone marrow edema characteristics, and the presence or absence of structural lesions rather than relying on bone marrow edema presence alone,” Bressem and colleagues wrote. “These findings could inform future consensus discussions on imaging criteria for axial spondyloarthritis.”
One reason for undertaking the study was that SBME’s prevalence in the general population hasn’t been established reliably. Bressem and colleagues found estimates in the 12% to 17% range in previous studies, neither of which drew from the population at large but instead focused on healthy and/or younger individuals. Meanwhile, other studies examining women postpartum and recreational runners found high rates of SBME, “suggesting that mechanical stress and hormonal changes can produce bone marrow edema indistinguishable from inflammation,” the authors wrote, adding that “comprehensive data from an unselected general adult population remain sparse.”
Having access to the German National Cohort was a great boon to the researchers. It’s one of the largest prospective, population-based studies ever conducted in which a substantial proportion underwent whole-body MRI scans. Some 205,000 Germans were enrolled in the overall cohort, of whom more than 11,000 had the scans. About 1,000 of these were read by human experts and the rest by the AI algorithm.
Mean participant age was 53 and just under half were women. About 24% had some history of chronic back pain and 15% reported experiencing it in the past year. However, only 0.5% had a formal axSpA diagnosis. In these and most other respects, the cohort resembled the general German population as characterized in previous studies.
Bressem and colleagues reported findings separately for the participants whose images were read by humans versus the AI system. Numerical findings were similar between the two groups, including for participants’ baseline characteristics as well as their risks for SBME. The main difference was that confidence intervals were narrower in the AI analysis, owing to the 10-times greater sample size.
Some of the subgroup findings on SBME risk based on the human-read images for all participants were as follows:
- Female vs male: OR 1.43 (95% CI 1.09-1.89)
- Age: OR 1.28 per 10-year increment (95% CI 1.14-1.46)
- Physical activity on the job: OR 1.39 (95% CI 1.06-1.83)
Subgroup results for female participants only showed statistical significance in the AI analysis, but the point estimates were generally similar for human-read images. Age and on-the-job physical activity were also predictors of SBME. History of any pregnancy raised the risk 40% (59% in the AI analysis) compared with nulliparous women, with a similar increase for those going to term.
Intensive recreational activity didn’t increase SBME rates among women, nor among men whose images were read by humans. The AI analysis, however, did show a significant increase in male athletes (OR 1.23, 95% CI 1.08-1.40).
The AI system seemed to be very accurate and reliable, the investigators concluded. Measures of its performance versus human readers indicated good concordance even when analyzed at the pixel level.
Ultimately, Bressem and colleagues concluded, their study demonstrates that SBME is far from definitive proof of axSpA; rather, they wrote, the findings “indicate that most bone marrow edema reflects mechanical stress and physiological adaptation rather than inflammatory disease.”
Source link : https://www.medpagetoday.com/rheumatology/arthritis/121188
Author :
Publish date : 2026-05-08 20:54:00
Copyright for syndicated content belongs to the linked Source.