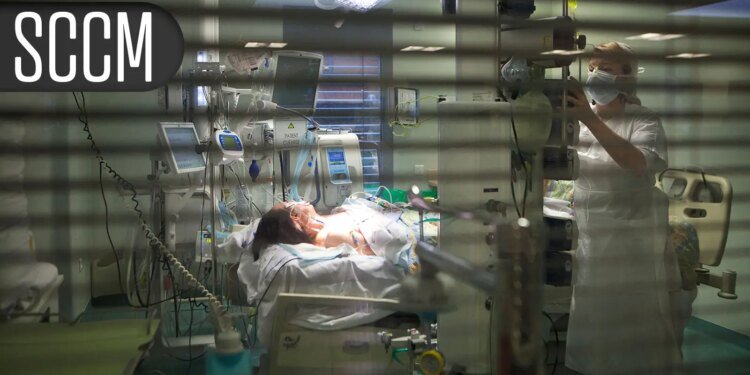
CHICAGO — Using endotracheal tubes (ETTs) coated with ceragenins did not reduce the incidence of ventilator-associated pneumonia (VAP) compared to standard subglottic suction ETTs, but mortality was lower with the ceragenin-coated ETTs, according to the CEASE VAP study.
In the prospective, pragmatic crossover trial, VAP occurred in 19% of patients receiving ceragenin-coated (Cerashield) endotracheal tubes (CSA ETTs) and 15% of patients receiving standard subglottic suction ETTs (SSETTs), a non-significant difference (RR 1.22, 95% CI 0.7-2.13, P=0.4), reported John Muscedere, MD, of Queen’s University in Kingston, Ontario, Canada, at the Society of Critical Care Medicine annual meeting. The findings were simultaneously reported in Critical Care Explorations.
However, mortality was lower in the CSA ETT group both in the ICU (20% vs 36% with SSETTs, P=0.01) and in the hospital overall (25% vs 43%, P=0.004). Patients on CSA ETTs also saw more ventilation-free days and there was a hint at a difference in antibiotic-free days, the researchers said.
The “intriguing” improved clinical outcomes, despite no difference in VAP incidence, are of “unknown significance and need to be confirmed,” Muscedere stated. “We were severely underpowered because of the numbers that we recruited, but our findings related to acceptability, safety, and implementation logistics support the conduct of a future multicenter cluster randomized study.”
VAP is estimated to occur in about 10-20 cases per 1,000 ventilator days, and prolongs mechanical ventilation approximately 7 days, as well as ICU stays approximately 8 days, Muscedere explained. ETTs act as conduits for VAP via the cuff and biofilm formation. Ceragenins — small molecules that mimic antimicrobial peptides — have previously shown effectiveness in preventing biofilm formation and reducing bacterial colonization.
The researchers compared patient outcomes from CSA ETTs to SSETTs in a pilot study to assess the feasibility of a randomized controlled trial. After a 6-week run-in period, the hospital alternated use of SSETTs and CSA ETTs in patients using a deferred consent model.
The hospital first used CSA ETTs for 11 weeks starting in February 2023 and then had a 2-week washout period before switching to SSETTs for 11 weeks. After another 2-week washout period, they used CSA ETTs for 12 weeks, followed by a 2-week washout and then SSETTs for 12 weeks.
The 63 patients in the run-in period received SSETTs. During crossover, 100 patients received the CSA ETTs and 160 patients received the SSETTs. The patients in all three groups had a similar average age (57-61) and did not significantly differ in sex, height, weight, primary diagnosis, morbidity scores, APACHE II scores, or receipt of vasopressors, dialysis, or antibiotics. The clinical frailty score was significantly lower in the CSA ETT group (3.5 on the Clinical Frailty Scale) than in the run-in SSETT and SSETT groups (3.9).
The number of VAPs per 1,000 ventilator days was 28.6 in the CSA ETT group and 22.4 in the SSETT group (RR 1.28, 95% CI 0.73-2.23, P=0.39). Though that difference was not significant, there were several significant differences in the secondary patient outcomes.
The average number of ventilation-free days was higher in the CSA ETT group (15.6 days) than the SSETT group (12.5 days, P=0.04).
The difference in average antibiotic-free days between patients with CSA ETTs (14.7 days) and those with SSETTs (11.8 days) just missed significance (P=0.047). The groups did not significantly differ in the percentage of patients who needed a new antibiotic more than 48 hours after ICU admission, the duration of mechanical ventilation, or the duration of ICU or hospital stay.
Respiratory cultures revealed that the incidence of pneumonia within 48 hours of intubation was not significantly different between the CSA ETT group (18%) and the SSETT group (11%, P=0.09). But the researchers did identify three specific pathogens whose incidence was significantly different between the groups.
The SSETT group had more Pseudomonas species (6% vs 0%, P=0.02) than the CSA ETT group, but the CSA ETT group had more Staphylococcus species (8% vs 3%, P=0.04) and more fungi/yeast species (12% vs 3%, P=0.01).
Muscedere’s group wrote that a study strength was “its real-world implementation in a high-acuity ICU setting without protocolized interventions, reflecting actual clinical practice leading to increased generalizability,” although they acknowledged the “inability to blind the study due to obvious inherent differences between the CSA ETT and the SSETT,” was a limitation that “may have impacted the results and introduced bias.”
Snigdha Jain, MD, MHS, of the Yale School of Medicine in New Haven, Connecticut, noted to MedPage Today that the “discordance between the null primary outcome and favorable secondary patient-centered outcomes may reflect surveillance-related overdiagnosis of VAP in the intervention arm or residual differences in some baseline risk factors, such as frailty and severity of illness.”
Still, “the findings raise the possibility that modifying airway biology may improve clinically meaningful outcomes and warrant further study,” said Jain, who was not involved in the study.
Miriam Treggiari, MD, PhD, MPH, also of Yale, and colleagues conducted a different clinical trial on VAP that similarly showed no impact on VAP incidence, but did not show the lower mortality in the CEASE VAP intervention group. Treggiari, who was not involved in the current study, advised caution when interpreting the results.
“The period-based, non-randomized design of CEASE-VAP, along with its smaller sample size, increases susceptibility to bias and limits the reliability of mortality comparisons,” Treggiari told MedPage Today. “Plausible explanations for the mortality differences are likely due to higher sources of bias in the CEASE-VAP study, including population selection, lack of patient-level randomization, secular trends, evolving clinical practices, and residual confounding, resulting in a spurious survival benefit.”
Source link : https://www.medpagetoday.com/meetingcoverage/sccm/120541
Author :
Publish date : 2026-03-28 14:42:00
Copyright for syndicated content belongs to the linked Source.