- GLP-1 medications may not always be effective for everyone.
- New research suggests that around 10% of people carry genetic variations that explain why.
- A new review suggests that certain combination approaches for obesity pharmacotherapy may be effective when GLP-1 drugs are not.
- Experts share recommendations for alternative weight loss strategies.
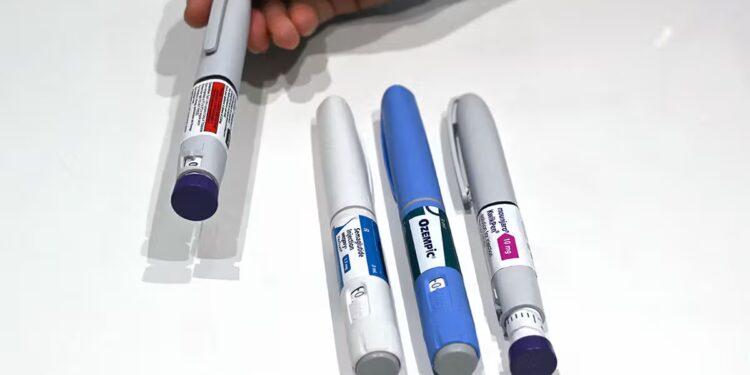
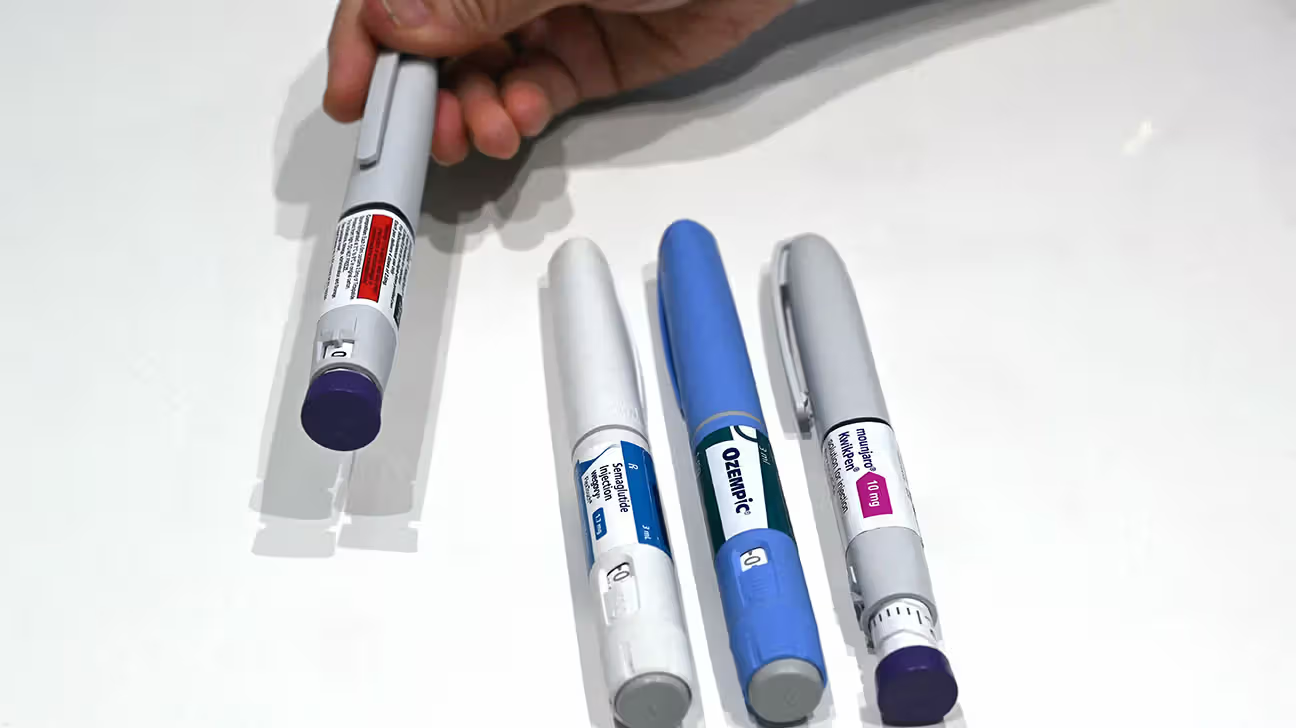
GLP-1 medications have exploded in popularity to manage type 2 diabetes and treat obesity.
The popularity of this class of medications, which includes Ozempic and Wegovy, is partly due to their widespread success for weight loss.
However, new research published in Genome Medicine shows that GLP-1 drugs may not be effective for everyone. The findings suggest that certain genetic factors may offer an explanation.
Around 10% of people carry genetic variations linked to “GLP-1 resistance.” These individuals appear to have higher-than-normal levels of the hormone glucagon-like peptide-1 (GLP-1). GLP-1 helps to regulate blood sugar. In contrast, the hormone appears less effective despite higher GLP-1 levels.
“This aligns with my clinical experience, where I frequently see a variable response to GLP-1 medications,” said Mir Ali, MD, bariatric surgeon and medical director of MemorialCare Surgical Weight Loss Center at Orange Coast Medical Center in Fountain Valley, CA. Ali wasn’t involved in the study.
It’s unclear whether these genetic variations influence weight loss. GLP-1 drugs are generally prescribed at higher doses for weight loss than for diabetes management. The current study focused on how GLP-1s and these genetic variants influence blood sugar levels.
The study focused on two genetic variants that affect the enzyme peptidyl-glycine alpha-amidating monooxygenase (PAM).
PAM plays a role in activating various hormones, including GLP-1.
Certain variants of PAM are more common in those with diabetes and may impair the release of insulin from the pancreas. The research team sought to determine whether these variants also disrupt GLP-1.
In addition to helping regulate blood sugar, GLP-1 also stimulates insulin release after meals, slows stomach emptying, and reduces appetite. GLP-1 drugs are made to mimic the effects of this hormone.
When the research team analyzed individuals with a PAM variant called p.S539W, they expected to find lower GLP-1 levels. However, they found elevated levels of GLP-1 in these individuals.
They also found that, even with higher GLP-1 levels, participants did not reduce their blood sugar levels more quickly. More GLP-1 was needed to achieve the same biological effect, indicating the participants were GLP-1-resistant.
“These findings support the idea that some patients may have partial biologic resistance to incretin-based therapies,” said Robert Glatter, MD, attending physician in the Department of Emergency Medicine at Lenox Hill Hospital in New York City, and Assistant Professor of Emergency Medicine at Zucker School of Medicine at Hofstra/ Northwell. Glatter wasn’t involved in the study.
“Still, genetics explains only a portion of treatment heterogeneity, and routine pharmacogenomic screening is not yet ready for widespread clinical use,” he added.
More research is needed to verify the effects genetic variations can have on weight loss with GLP-1s. Still, the findings show promise for the future of obesity treatment.
“The broader lesson from recent research is that obesity treatment is entering a precision-medicine era,” Glatter said. “Instead of asking whether GLP-1 medications work, clinicians are beginning to ask for whom they work best — and what alternative pathways should be considered when responses are incomplete.”
We asked our experts to explain why GLP-1s don’t always work for weight loss and what alternatives are available. These interviews have been lightly edited for clarity.
What other factors influence GLP-1 effectiveness?
Ali: Other factors can include underlying medical conditions or the patient not using the medications exactly as prescribed.
Glatter: In practice, many patients labeled “non-responders” to GLP-1 therapy are experiencing incomplete dosing, early discontinuation because of gastrointestinal side effects, insufficient treatment duration, or competing metabolic drivers such as severe insulin resistance, sleep disruption, sarcopenia, or medication-associated weight gain.
Addressing these contributors often restores treatment effectiveness.
What other options do people have if GLP-1s don’t work?
Ali: If a patient meets the criteria, surgical weight loss remains the most effective long-term solution.
Glatter: Another important option that deserves earlier consideration—not later referral—is metabolic and bariatric surgery. Too often framed as a last resort after medication failure, surgery is better understood as a parallel therapeutic strategy within the same treatment continuum.
Procedures such as sleeve gastrectomy and Roux-en-Y gastric bypass produce average weight reductions of 25 to 35% and remain the most durable interventions available for severe obesity and obesity-related metabolic disease.
Importantly, surgery also alters incretin signaling itself, increasing GLP-1 activity and improving insulin sensitivity in ways that complement pharmacologic therapies.
Is combination pharmacotherapy an option?
Glatter: When response remains limited despite optimization, clinicians should consider moving beyond monotherapy.
Obesity is a network disease involving appetite regulation, reward signaling, gut-brain hormones, and energy expenditure pathways.
Ali: If surgery is not an option, we can try medications that stimulate more than one receptor (such as Zepbound) or a combination of different medications.
What are some other proven weight loss strategies?
Ali: The majority of weight loss is driven by dietary modifications—primarily reducing carbohydrate and sugar intake while emphasizing proteins and vegetables. Adding both aerobic and resistance exercise further helps burn calories and mitigate muscle loss.
Glatter: Additional approaches to lose weight and manage cardiometabolic aspects of obesity include adherence to the Mediterranean, DASH, or MIND diet, along with adequate strength training, close monitoring of hydration status, and caloric intake to maintain and prevent muscle loss, particularly while taking a GLP-1.
Even if one chooses not to take a GLP-1 to manage weight loss, adherence to a Mediterranean-style diet, adequate hydration, and resistance training combined with aerobic exercise is recommended for weight loss and preservation of muscle mass.
Source link : https://www.healthline.com/health-news/glp-1-effectiveness-ozempic-wegovy-varies-based-on-genetics
Author :
Publish date : 2026-04-14 10:52:44
Copyright for syndicated content belongs to the linked Source.